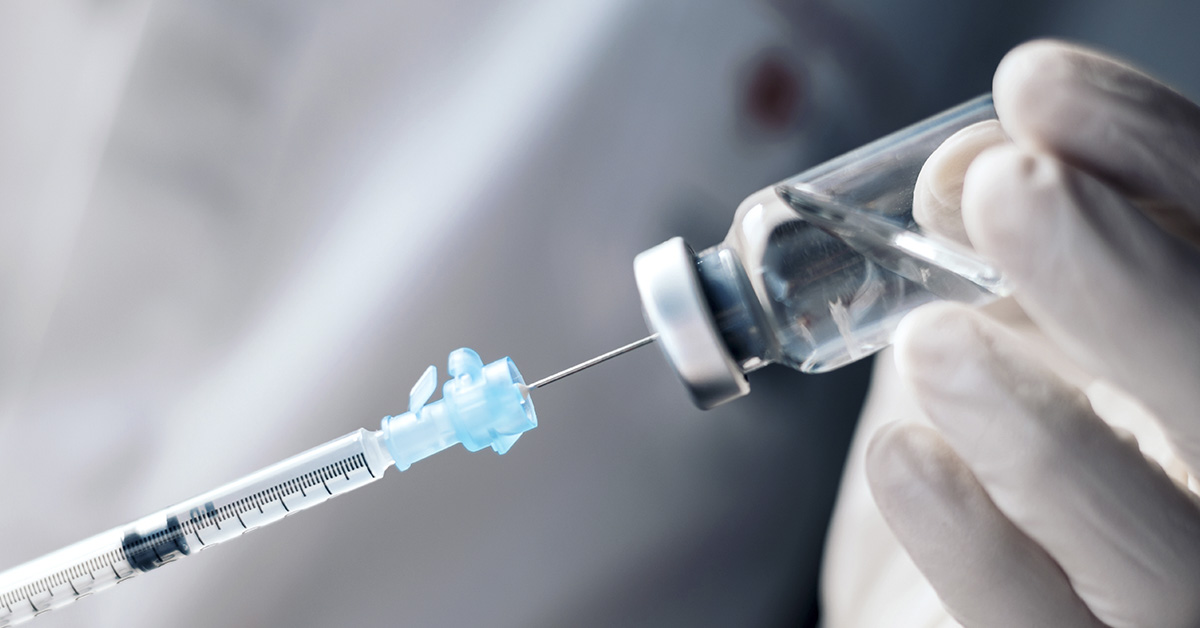
Headlines in mid-December 2025 suggested the FDA was considering its strongest label language for COVID-19 vaccines. Yet follow-up reporting indicated that FDA leadership had no plans to add a boxed warning, or “black box,” warning. That swing is significant because a boxed warning is a high-impact signal to clinicians and patients. It can change how shots are discussed, how often they are given, and how risks are explained. It also occurs at a tense moment in vaccine policy, when agencies are re-evaluating safety claims and the public is awaiting clear evidence. This article explains what a boxed warning is, what COVID-19 vaccine labels already say, and what the best-sourced safety systems can, and cannot, prove. It also lays out what to watch for next, because the key issue is not a rumor. The key issue is whether the FDA publishes data, methods, and a reasoned labeling decision.
What was reported, and what is known as of December 2025
Reports first said the FDA “intends” to add a boxed warning, citing people familiar with internal plans. Those accounts described a focus on rare heart inflammation, especially myocarditis, and the possibility of stronger language for certain groups. Reuters also reported that the plan was not finalized and could still change. Then, on December 15, 2025, Reuters reported a different message. It said FDA Commissioner Marty Makary told Bloomberg the agency had no plans to add a boxed warning.
In that same Reuters report, Makary linked more frequent dosing to higher side-effect rates, and he suggested annual dosing may differ. This implies that the internal debate may involve both risk level and dosing strategy. One important detail is that “considering” a boxed warning is not the same as issuing one. It is also not the same as adding standard warnings, which COVID-19 vaccine labels already include. Officials themselves cautioned that claims about a decision, before an FDA announcement, are speculation. As HHS spokesperson Andrew Nixon put it, “Unless the FDA announces it, any claim about what it will do is pure speculation.”
What a “black box” warning actually means in FDA labeling
A boxed warning is the FDA’s most prominent warning format for prescription products, placed in a bordered box near the top. It is designed to force attention to a serious risk or a major restriction on use. Unlike a news headline, the label is a legal document, and wording choices carry consequences for clinicians and manufacturers. The FDA also has internal standards for how these sections should be written. In its labeling guidance, the agency says the goal is consistency and clarity for prescribers and patients. The guidance states that the recommendations are meant to help ensure labeling is “clear, useful, informative.” This isimportant, because the argument for a boxed warning must clear a high bar. The FDA has to believe the risk message needs the strongest possible placement.
It is also worth separating terms. “Black box” is a common media phrase. The FDA’s formal term is “boxed warning.” The practical effect is the same. The message becomes hard to miss in prescribing information, and it can drive changes in clinical practice. In real life, doctors may respond by spacing doses differently, screening more carefully, or avoiding the product for certain patients. So the right question is not whether boxed warnings are rare in medicine. The right question is whether COVID-19 vaccine risks meet the FDA’s threshold for that format, given what is already on the label.
What COVID-19 vaccine labels already warn about today

COVID-19 vaccine labels have warned about myocarditis and pericarditis for years, especially for mRNA vaccines. In June 2025, the FDA announced updated label language that added more detail, including estimated incidence ranges after a specific seasonal formula. This reveals that the FDA was already using labeling to sharpen risk communication, without a boxed warning. The FDA’s June 2025 page includes a concrete estimate that has been widely cited in coverage. It states the “estimated unadjusted incidence” in males 12 through 24 years was “approximately 27 cases per million doses” in the 1 through 7 day window after vaccination.
It also notes that MRI findings suggesting myocardial injury were common in a follow-up study, while adding that the “clinical and prognostic significance” of those MRI findings is not known. That language is careful for a reason. It communicates a real risk, puts a number on it, and admits uncertainty about the longer-term imaging meaning. It also signals that the FDA is looking beyond acute hospital discharge outcomes. At the same time, the CDC’s clinical page describes myocarditis after vaccination as rare, with many cases resolving by discharge. If the FDA were to move from these warnings to a boxed warning, it would be saying the current placement and emphasis are not enough.
How safety signals are detected, and why VAERS alone cannot prove causality
A lot of the current controversy turns on how post-market signals are found and validated. VAERS is one of the first places signals can appear, because it is open to reports from the public and clinicians. That openness is a strength for early detection, but it is also the reason VAERS cannot settle cause and effect on its own. HHS’s VAERS data page makes the limitation explicit. It says, “The number of reports alone cannot be interpreted as evidence of a causal association.”It also warns, “Reports may include incomplete, inaccurate, coincidental, and unverified information.”
The CDC repeats a similar point, stating, “A VAERS report alone does not indicate whether a vaccine caused or contributed to an adverse event.”That is why strong claims about deaths “caused by” vaccines require more than VAERS counts. The normal pathway is signal, then deeper review using medical records, active surveillance systems, and targeted studies. The FDA itself notes that if a signal is found, “further studies” can be done in systems such as the Vaccine Safety Datalink. So, if a boxed warning is ever proposed, the key evidence should be the kind of investigation that moves beyond raw reports and toward confirmed case definitions and causal inference.
Myocarditis, dosing intervals, and what the agencies are debating
Myocarditis and pericarditis are now well-described adverse events associated with mRNA COVID-19 vaccination, especially in adolescent and young adult males. The CDC says evidence from multiple monitoring systems “supports a causal association” between mRNA vaccines and myocarditis and pericarditis. That sentence is important because it is stronger than “reported after.” It is the CDC stating the association is causal, while still emphasizing rarity. The FDA’s June 2025 update adds granularity about timing and incidence. It also highlights uncertainty about the meaning of persistent MRI abnormalities at about 5 months. The blend of numbers and uncertainty is typical for labeling science, and it creates space for debate over what warning format is proportionate.
Reuters reported that Makary, in a Bloomberg interview, said “Giving two doses of the vaccine just 3 months apart was linked to higher rates of side effects.”If dosing spacing is part of the argument, then the FDA’s final position could be narrower than many headlines imply. It could focus on schedule guidance, specific age bands, or product classes, not a sweeping boxed warning. Clinically, the message to patients stays the same in the meantime. Chest pain, shortness of breath, and palpitations after vaccination need evaluation, especially in younger people. Risk communication works best when it is specific, time-bound, and linked to action.
What manufacturers and recent evidence say about the benefit-risk
Manufacturers have pushed back against the implication that new safety problems have emerged. Reuters reported Pfizer reiterated that its vaccine continues to show a “favorable safety and efficacy profile supported by extensive real-world evidence.” Pfizer’s own September 2025 update on its 2025–2026 formula described trial results and said, “The safety profile of the vaccine was consistent with previous studies, with no new safety concerns identified.” Those statements do not erase myocarditis risk, and they do not replace independent surveillance. However, they help explain why a boxed warning would be a major escalation. A boxed warning communicates that a risk is not only real but significant enough to require the strongest label placement.
That is a different regulatory signal than adding incidence numbers to existing warnings. This is where the FDA’s role is specific. It is not asked to argue a political case. It is asked to weigh benefits and risks for defined populations, based on evidence that can be audited. If the agency believes risk is being underestimated for a group, it can restrict indications, adjust schedules, update warnings, or require new studies. If the agency believes current warnings already communicate the relevant risk, then a boxed warning may be judged unnecessary, which is what the December 15 reporting suggested.
Communication risks: why warning language can change behavior fast

Label changes do not stay inside medical journals. They spread through headlines, social media, and everyday conversations at clinics. That is why experts worry about what happens when the strongest warning is floated without published supporting work. In the SAN report, vaccine researcher Michael Osterholm was quoted as saying, “It’s irresponsible science at best, and it’s dangerous to the public at the very least.” A boxed warning can be interpreted by the public as “this product is unsafe,” even when the real message is narrower. It can also cause some people to ignore the underlying issue, because messaging becomes tribal. Both outcomes harm decision-making. Clear labeling should support informed consent, not amplify confusion.
There is also a trust issue inside medicine. If clinicians think the label is being used as a political instrument, they may discount it. If patients think agencies hide uncertainty, they may discount everything. Neither is good for public health, especially for older adults and high-risk patients who still benefit most from updated protection. So the communication standard should be simple. If the FDA believes a boxed warning is justified, it should publish the evidence and reasoning. If it does not, it should clearly explain why the current warnings are sufficient.
Read More: Study Suggests Possible Link Between Pfizer COVID-19 Vaccine and Vision-Related Eye Conditions
What patients and clinicians should do while the debate continues
Until the FDA publishes an official labeling action, people should treat“boxed warning coming” claims as unconfirmed. At the same time, people should take the known myocarditis risk seriously because the CDC and FDA both acknowledge it, and both agencies give practical clinical steps. For clinicians, the CDC guidance is straightforward. “Consider myocarditis and pericarditis in persons with acute chest pain, shortness of breath, or palpitations,” especially in adolescents and young adults.
It also recommends reporting cases to VAERS, because signal detection still depends on reporting.For patients, the safest approach is personal, not viral. Discuss your age, prior doses, infection history, and heart history with a clinician who can interpret risk. If you recently got vaccinated and develop concerning symptoms, seek care quickly. Most myocarditis cases reported after mRNA vaccination have improved by discharge, but prompt evaluation is still the smart move. Finally, watch for the concrete signals of a real policy change. Those are updated FDA prescribing information, an FDA safety communication, and posted evidence, not anonymous sourcing.
Conclusion
The story of a possible COVID-19 vaccine boxed warning moved quickly in December 2025. Early reporting described an intent to add the strongest label warning. Days later, reporting said FDA leadership had no plan to do so. That shift does not remove the underlying safety issue. Myocarditis and pericarditis after vaccination are real, and agencies already warn about them. The central problem is evidence discipline. VAERS can surface signals, but it cannot prove causation by itself. A boxed warning, if ever used, should rest on transparent methods and verified data.
The FDA has the tools to do that work, and the public has the right to see it. Until an official label change is published, the practical guidance stays steady: take chest symptoms seriously, report suspected cases, and make vaccine decisions with a clinician who can weigh your individual risk. Clear communication, published evidence, and consistent standards remain essential, especially when policy debates unfold in public view and influence personal medical decisions across different age groups and risk profiles.
Disclaimer: This information is not intended to be a substitute for professional medical advice, diagnosis or treatment and is for information only. Always seek the advice of your physician or another qualified health provider with any questions about your medical condition and/or current medication. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.
A.I. Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.
Read More: University Researchers Report Progress Toward Universal Cancer Vaccine