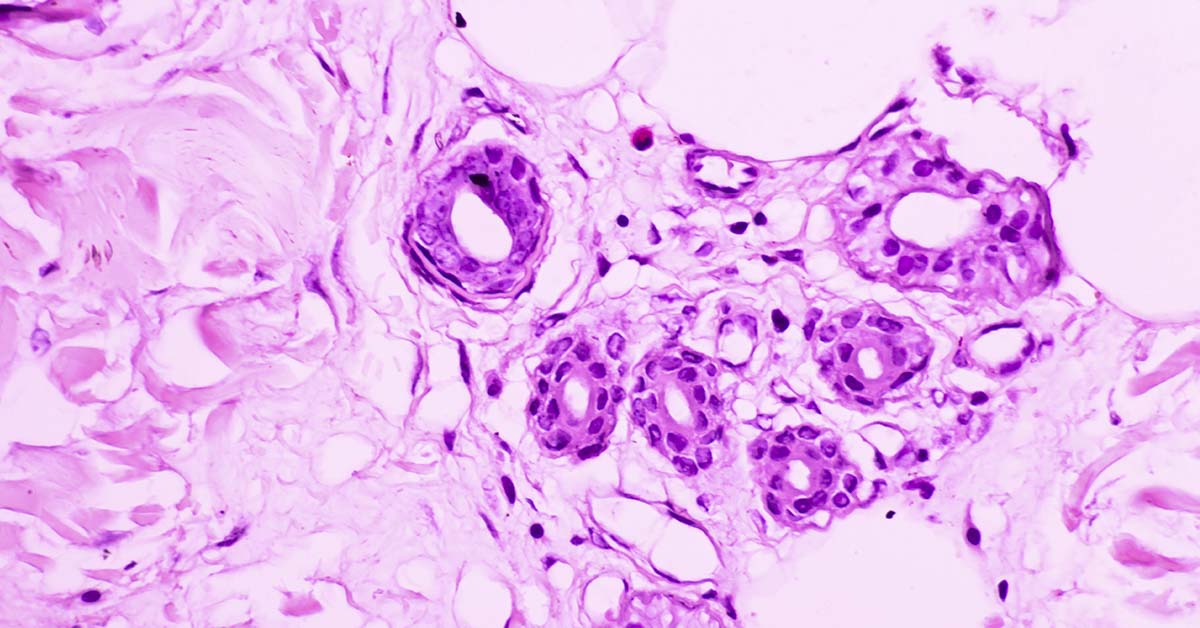
When a patient’s cancer goes into remission, their tumor cells stop growing, and their symptoms improve. This remission period can persist for many years, with both the cancer cells and the microclimate around the tumor helping to keep the cancer inactive. However, inflammation can disturb this environment and reactivate the dormant cancer cells. This process can lead to metastasis, where the cancer starts to spread, although scientists still don’t completely understand why this occurs.
How Viral Infections Could Be Activating Dormant Cancer Cells

Julio Aguirre-Ghiso works as a cancer biologist at the Albert Einstein College of Medicine in New York City. During the first couple of years of the COVID-19 pandemic, he noticed an increase in cancer deaths. Aguirre-Ghiso had his suspicions that dormant cancer cells may be activated by viral infections. Working together with researchers from Utrecht University and the University of Colorado, the team revealed that inflammation resulting from viral infections could activate the dormant cancer cells and trigger metastasis. Their findings were published in Nature and offer significant insights for clinicians around the world regarding cancer remission.
Reigniting the Embers of Cancer

In a press release, a coauthor of the study, cancer geneticist James DeGregori, stated that “Dormant cancer cells are like the embers left in an abandoned campfire, and respiratory viruses are like a strong wind that reignites the flames.” The researchers used mice with two types of breast cancer that had dormant cancer cells. They then infected the mice with either the mouse-adapted COVID-19 virus or influenza A. The researchers found that after three to 15 days of being infected, the number of metastatic cells increased and remained high for nine months.
Changes Caused By Activation of Dormant Cancer Cells
When the dormant cancer cells became active again, it led to changes to their surface proteins and gene expression. These cells started to show signs typically observed in active cancer, such as the expression of epithelial markers and genes linked to the formation of new blood vessels. These changes are typically observed when the cancer is once again growing and spreading across the body. To learn more about how this activation occurs, the researchers looked at the inflammatory cytokine interleukin 6 (IL-6), which is usually produced in the early stages of a viral infection. Compared to normal mice, mice that were deficient in IL-6 exhibited less cancer cell activation and metastasis.
Looking for Other Immune Factors
IL-6 levels drop after the early stage of an infection, so the researchers examined other potential immune factors that may maintain the active status of the cancer cells. The team discovered that removing CD4+ T cells resulted in fewer reactivated cancer cells after infection and an increase in cancer-killing CD8+ T cells in the lungs. Therefore, they believe that the CD4+ T cells were actually preventing the CD8+ T cells from entering the tissue. They found that the reawakened cancer cells were changing the CD4+ T cells in a manner that made them limit the CD8+ T cells’ activity.
The Link Between COVID-19 Infections and Cancer Deaths
For the final step of this study, the team used two different datasets to examine the connection between COVID-19 infections and cancer deaths. They found a correlated increased risk of deaths in the months after a COVID-19 infection. In the press release, Aguirre-Ghiso added that, “Our findings indicate that individuals with a history of cancer may benefit from taking precautions against respiratory viruses, such as vaccination when available, and discussing any concerns with their healthcare providers.”
Changes In Cancer Remission Monitoring

The findings of the study could lead to major changes in how cancer patients in remission are monitored. For example, doctors could start looking more closely at survivors’ immune responses after viral infections to consider early interventions that could prevent dormant cancer cells from reactivating. Additionally, targeting specific immune cells (such as CD4+ T cells) could be used as a new way to prevent cancer from coming back after remission.
More Studies and Research Needed

While this study has revealed some significant findings, more studies are needed to find out how the immune system and viruses interact with dormant cancer cells. If we can better understand these complex relationships, we may be able to create new therapies that prevent cancer reactivation before it even begins. The latest findings also suggest that existing anti-inflammatory treatments and vaccines could potentially play a role in reducing the recurrence of cancer in those most vulnerable.
The Bottom Line

Being a cancer survivor is challenging enough on its own. Having to deal with the possibility of dormant cancer cells reactivating must certainly add even more stress to a patient’s life. This study has revealed that common respiratory infections could potentially do just that – reactivating cancer cells that have lain dormant for years. Hopefully, this new information will lead to new methods of prevention and care. With a better understanding of the mechanisms that drive this process, we may be able to reduce patients’ chances of their cancer returning.
Read More: Deadly Brain Tumor Disappears After Experimental Cancer Treatment