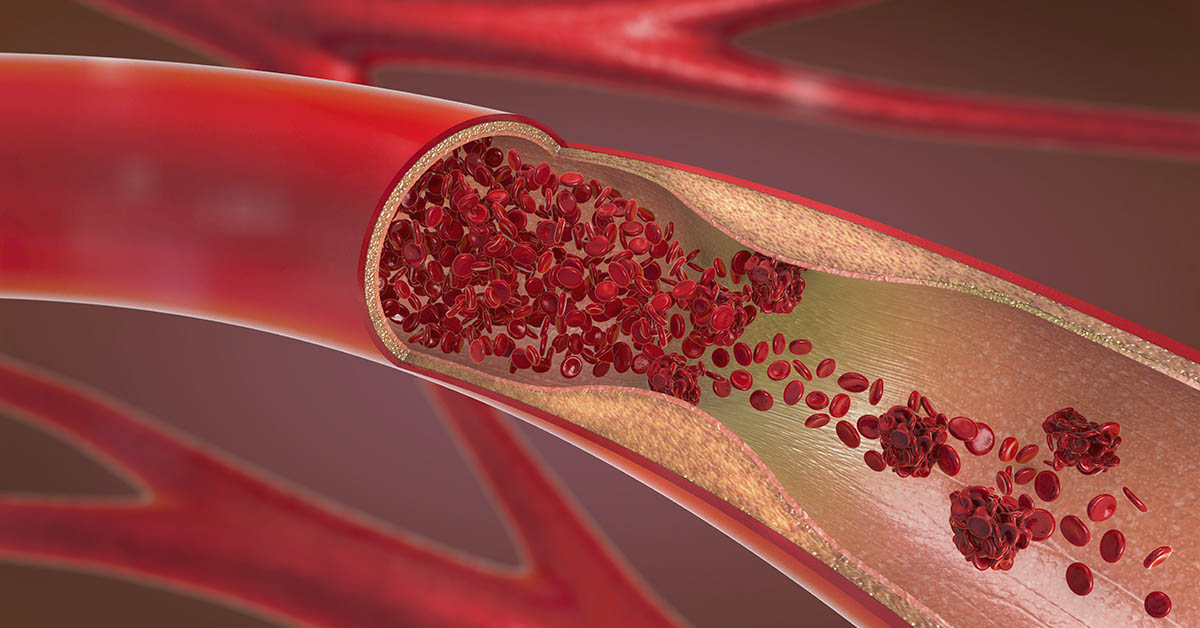
Blood clots help the body stop bleeding after an injury, which is a normal and protective response. However, a clot becomes dangerous when it forms inside a vein or artery without a cut or wound. In these cases, the clot can narrow a blood vessel and slow circulation. It can also block blood flow entirely, which raises pressure inside the vessel. This blockage can injure nearby tissue and place added strain on the heart. A clot that forms in a deep vein is called deep vein thrombosis, or DVT. Many DVTs begin in the legs, although clots can form elsewhere in the body as well. If part of a clot breaks away and travels to the lungs, it causes a pulmonary embolism, or PE. PE can become life-threatening very quickly. The challenge is that early warning signs often seem quite ordinary. People commonly assume a cramp, a muscle strain, or simple travel stiffness. Some people notice very little until the situation suddenly worsens.
The CDC notes that DVT and PE symptoms can be non-specific, which adds to confusion and delay. Therefore, knowing what to watch for becomes especially important. This awareness is important after long periods of sitting, recent illness, surgery, injury, pregnancy, or hormone use. Awareness does not mean panic or self-diagnosis. However, it does improve response time. People who recognize concerning changes often seek medical care sooner. Earlier evaluation can reduce complications, limit clot growth, and lower mortality risk. Education also supports informed decisions, clearer conversations with clinicians, and faster access to testing when symptoms cluster or escalate rapidly.
Leg cramps that do not act like a normal cramp

A DVT in the leg often starts with pain that sounds ordinary at first. Many people describe a deep cramp in the calf. Others notice soreness behind the knee. Some people also report a dull ache in the thigh. The level of concern rises when pain affects only 1 leg. It also rises when the pain has no obvious cause. Symptoms may begin after long travel, extended desk work, or bed rest. Many people assume dehydration or overuse. As a result, they try water, stretching, or a hot shower. Those steps can help with a true muscle cramp. However, they may not help when a clot is driving the pain. The National Blood Clot Alliance describes a classic clue: “Leg pain or tenderness often described as a cramp or charley horse.” This wording matters because it closely matches how many patients describe early DVT symptoms.
A typical muscle cramp often improves after walking and stretching. In contrast, a DVT-related cramp can return throughout the day. It can also remain sore between episodes. Pain may increase when standing or walking for longer periods. Additionally, some people notice a sense of heaviness in the same leg. Others notice tenderness along a visible vein line. The CDC travel medicine guidance lists typical DVT signs as pain or tenderness, swelling, warmth in the affected area, and redness or discoloration of the overlying skin. Therefore, if leg pain appears alongside swelling or warmth, do not wait. Call a clinician and explain exactly what changed. Mention recent travel and how long you were seated. Also mention recent illness or bed rest. These details help with risk assessment. An ultrasound can confirm or rule out DVT quickly. Early treatment can significantly reduce the chance that a clot travels to the lungs.
Back, flank, or groin pain that appears without an injury

Back pain is common, so it is easy to brush off initially. Many people connect it with posture, lifting, or stress. However, clots can form in deeper veins inside the pelvis or abdomen. When this happens, pain can show up in the lower back. It may also appear in the flank or groin. Importantly, the pain can arrive without any clear injury. It may occur alongside thigh heaviness or leg swelling. Some people notice pain that worsens when standing. Others describe a tight, deep discomfort that does not match their usual back problems. Because back pain has many possible causes, people often wait several days. Unfortunately, that delay can be significant if a clot continues to grow.
Cleveland Clinic includes a clear reference to deeper clot pain. It lists: “Abdominal pain or flank pain may occur when blood clots affect the veins deep inside your abdomen.” Back or flank pain alone does not prove a clot. However, context changes risk. Think carefully about the last 2 weeks. Consider surgery, long immobility, or serious illness. Additionally, the CDC emphasizes that DVT and PE symptoms are nonspecific. Therefore, if back or flank pain appears with 1-sided leg swelling, warmth, or discoloration, seek medical advice promptly. Clinicians may first look for DVT in the leg. They may also consider clot locations higher in the body. Fast evaluation matters because treatment decisions depend on clot location and severity.
Skin discoloration on one limb
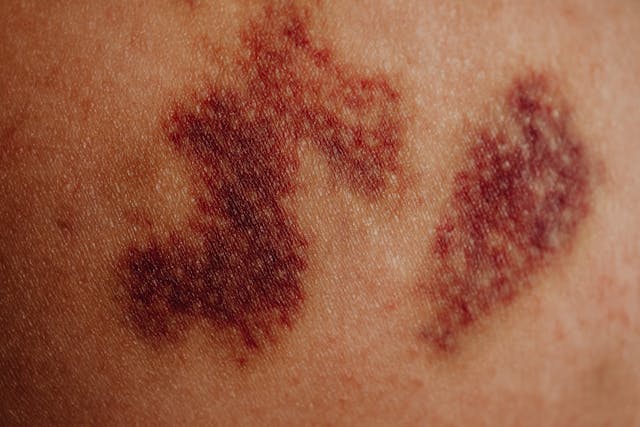
A clot disrupts normal circulation, and that disruption can change skin color where blood flow slows. Some people notice redness on the calf or thigh. Others notice darker tones or a bluish color change. The change may begin as a small patch. Over time, it can spread along the calf or around the ankle. People often assume bruising or irritation from clothing. Additionally, skin tone and lighting can make these changes harder to see. The key clue is asymmetry. One leg or arm looks different from the other. Concern rises when discoloration appears alongside pain, swelling, or warmth. These signs often appear together in DVT.
The NHS describes a specific warning sign: “red or darkened skin around the painful area.” The NHS also notes that this may be harder to see on brown or black skin. This detail matters because many people miss early color changes. The CDC also lists redness or discoloration among blood clot symptoms. Discoloration can also come from infection, dermatitis, or a bruise. A clinician can assess those possibilities. However, if discoloration persists beyond a day, seek evaluation. If it spreads quickly, seek urgent care. Do not rely on self-checks alone. A clot can injure veins and raise long-term risk if left untreated.
Warm skin over a painful area

Warmth is easy to ignore at first. People often assume a strain or minor inflammation. With DVT, warmth usually affects one limb. It often appears near the calf or behind the knee. It can also appear in an arm. This warmth comes from local inflammation around the clot. The area may also feel tender to the touch. Some people notice warmth only after comparing both legs. Warmth becomes more concerning when it lasts for hours. It matters even more when it appears with swelling, cramping pain, or discoloration. These combined signs should prompt medical review, because they fit the typical DVT symptom group.
NIH’s News in Health includes a direct expert description: “Deep vein thrombosis has classic symptoms, for example swelling, pain, warmth, and redness on the leg,” says Dr. Andrei Kindzelski. The same NIH article adds that about 30 to 40 percent of cases go unnoticed because symptoms may not look typical. This explains why warmth often gets missed. Therefore, if warmth persists and you also have a new cramp or swelling, call a clinician. Mention recent travel, bed rest, or surgery. These factors can increase risk by slowing blood flow. Avoid massage over a suspected clot area. Instead, let a clinician advise you, because treatment choices depend on proper assessment and imaging.
One-sided swelling in the leg or arm

Swelling is one of the most common clot signs. Yet many people dismiss it as water retention. Some assume salt intake caused it. Others blame standing or heat. DVT swelling often affects 1 leg. It may start at the ankle and move upward. Some people notice a tighter shoe on 1 side. Others notice a deeper sock mark. The calf may also look fuller than the other side. Arm swelling can also occur, although leg DVT is more common. Swelling may build over a day, or it may appear suddenly. It can also come with tenderness when pressing the calf. Some people notice discomfort when walking upstairs. These details help separate DVT from ordinary puffiness.
The NHS lists this symptom plainly: “swelling in 1 leg (rarely both legs).” The CDC also includes swelling among blood clot symptoms. Swelling has many causes, including injury and heart conditions. That is why evaluation matters. Clinicians often use ultrasound to check for DVT. The American Heart Association highlights that testing is straightforward, noting: “We can look with an ultrasound.” Therefore, if swelling occurs with pain, warmth, or discoloration, seek care promptly. If swelling occurs with shortness of breath or chest pain, treat it as an emergency. These can be PE symptoms, and delaying care can be dangerous.
Excessive sweating with chest or breathing problems

Sweating has many explanations, so it often gets ignored. Heat, anxiety, infection, and pain can all cause sweating. However, in clot emergencies, sweating can appear with pulmonary embolism. People may also have rapid breathing and a fast pulse. Some people look pale or clammy. Others feel lightheaded or close to fainting. These signs can appear even if leg symptoms were mild. Some people report a sudden wave of being unwell. They may also notice chest discomfort or upper back discomfort. The key issue is the combination. Sweating plus breathing changes suggest a serious problem, even if you are not doing anything physical at the time.
Cleveland Clinic lists “Excessive sweating” among pulmonary embolism symptoms. It also lists pale, clammy, or bluish skin. Sweating alone does not confirm PE. However, sweating with unexplained breathlessness is a serious warning. Therefore, seek urgent care, especially if symptoms start at rest. Do not drive yourself if you feel faint. A medical team can check oxygen, pulse, and blood pressure quickly. They can also order imaging when needed. Mayo Clinic warns that PE can be life-threatening and calls for urgent attention with key symptoms. Rapid care can prevent severe complications, including shock.
Shortness of breath, chest pain, or fainting

Shortness of breath is one of the most urgent clot signs. A clot in the lungs can reduce oxygen exchange quickly. Breathlessness may start with light activity. It can also start at rest. Many people also develop chest pain. The pain often worsens with a deep breath or cough. Some people cough up blood. Others faint or nearly faint. These symptoms can resemble asthma, pneumonia, panic, or a heart event. That overlap can delay care. When a clot blocks lung vessels, time matters. Treatment works best when care starts early. Even a small PE can become dangerous if it triggers low oxygen or heart strain.
The CDC gives clear instructions: “If you have any of these signs or symptoms, you should seek medical help immediately.” The CDC lists PE signs, including difficulty breathing, chest pain, coughing up blood, and fainting. It also lists very low blood pressure, lightheadedness, or fainting. Mayo Clinic adds: “Seek urgent medical attention if you experience unexplained shortness of breath, chest pain, or fainting.” Therefore, do not wait for symptoms to become severe. If you also have leg swelling or leg pain, tell the clinician. That connection can speed diagnosis and treatment.
Read More: Garlic and Blood Clots: Natural Support or Just Health Hype?
Other signs to look out for beyond the usual DVT clues

Blood clots do not only cause leg symptoms. They can also trigger warning signs when they affect the lungs, brain, heart, or surface veins. A pulmonary embolism can cause a fast or irregular heartbeat, sharp chest pain, coughing, or fainting. The CDC warns that “You can have a PE without any symptoms of a DVT.” Therefore, breathing trouble that starts without a clear cause deserves urgent care. A clot can also block blood flow to the brain and cause a stroke. The American Stroke Association lists sudden warning signs, including weakness on one side, trouble speaking, vision changes, balance problems, and a severe headache. If any of those appear, treat it as an emergency.
Some clots affect the heart and can be mistaken for indigestion or fatigue at first. Chest pressure remains common, yet the symptoms often vary widely. Mayo Clinic lists heart attack symptoms that include chest pain, pain spreading to the arm, back, neck, jaw, or upper belly, nausea, dizziness, fatigue, and cold sweat. One easy-to-miss sign is a cold sweat during chest discomfort. Mayo Clinic includes “Cold sweat” in its symptom list. Another clue can appear on the skin surface. A superficial vein clot can create a tender, red area, sometimes with a firm cord under the skin. Mayo Clinic notes that superficial thrombophlebitis symptoms can include warmth, redness, tenderness, and a cord-like vein change. If symptoms escalate quickly or involve breathing, speech, or fainting, seek emergency help immediately.
Conclusion
Blood clot symptoms get missed because they mimic common problems. A cramp can look like dehydration. Swelling can look like travel puffiness. Back pain can look like posture strain. Warm skin can look like a minor injury. Sweating can look like stress. A single symptom can mislead. However, clusters are more concerning. Two or more signs in 1 limb deserve quick attention. Risk factors also change urgency. The CDC notes that DVT and PE symptoms are nonspecific, which means they can resemble other conditions.
The CDC also states: “You can have a PE without any symptoms of a DVT.” Therefore, sudden breathlessness, chest pain, or fainting should trigger emergency care, even without leg symptoms. Prompt action saves lives and preserves long-term health. Treatment works best when started early. Delays increase damage to the veins and lungs. Trust physical warning signs. Seek evaluation without embarrassment or hesitation. Medical teams prefer early questions. Acting quickly protects mobility, breathing, and independence, while reducing anxiety through clear answers today.
Disclaimer: This information is not intended to be a substitute for professional medical advice, diagnosis or treatment and is for information only. Always seek the advice of your physician or another qualified health provider with any questions about your medical condition and/or current medication. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.
AI Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.
Read More: 12 Foods That Could Help Reduce Blood Clot Risk (And Some to Avoid)