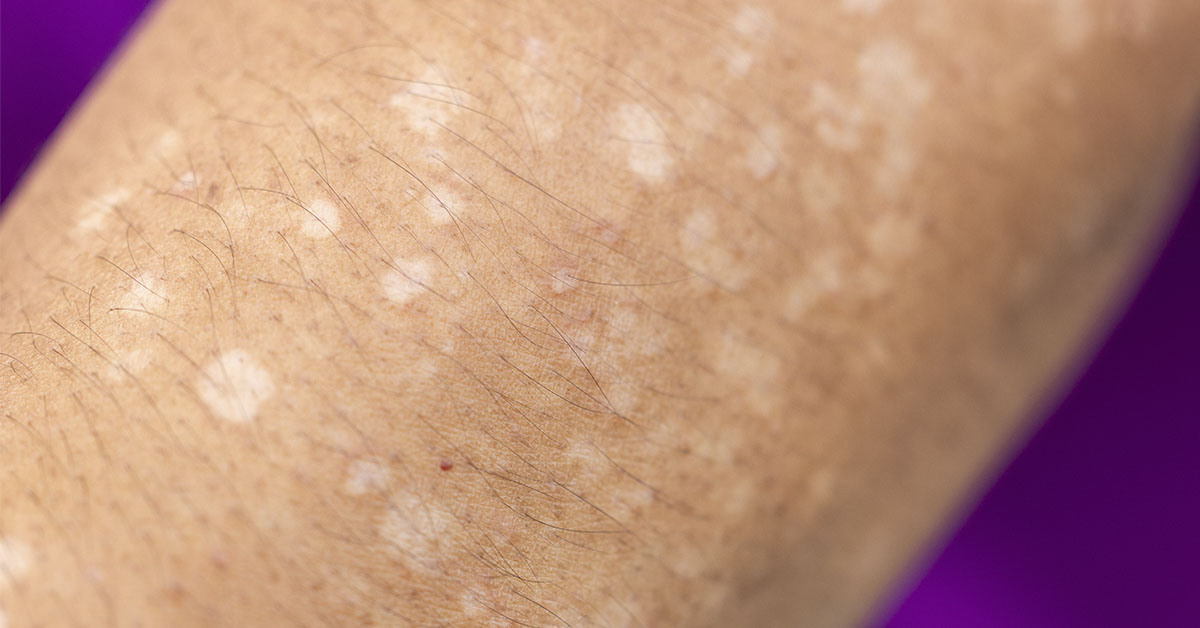
White spots on the skin can unsettle anyone, especially when they appear on bare arms or lower legs. They look simple, yet they rarely have one simple explanation. Some come from harmless surface yeast. Others follow dryness, irritation, or mild eczema. Still others appear after years of sun exposure. Others develop when the skin loses pigment completely. That range explains why internet searches often create more confusion than clarity. The phrase white spots on skin describes an appearance, not a diagnosis. The same is true for white spots on arms or white spots on legs.
A careful answer depends on several details. It depends on what the spots look like, where they sit, and how they change. Surface clues matter here as well. One slightly flaky patch tells a different story from a tiny pearly bump. Meanwhile, a sharply white area with crisp edges points in a different direction again. Once those differences are understood, the likely causes become much easier to sort. That is where the useful work begins. Instead of jumping to the worst possibility, it helps to read the clues the skin is already giving. The conditions below are among the most common explanations doctors consider first.
Not Every White Spot Tells the Same Story
The first job is to stop treating every pale mark as the same problem. Dermatologists do not begin with fear. They begin with shape, scale, texture, and location. The American Academy of Dermatology says white spots and patches develop “for many reasons.” That broad statement is the key to the whole subject. A tiny raised bump belongs in a different category from a flat patch. Meanwhile, a dry area suggests something different from a smooth one. Then a spot that appears after tanning tells its own story. When people search for what causes white spots on arms and legs, they often find several names at once. Those names can blur together quickly. In practice, the surface clues often separate them. If the skin carries fine scale, tinea versicolor or pityriasis alba becomes more likely.
When the area looks fully white and smooth, vitiligo rises higher. Meanwhile, a firm raised spot makes Milia a better fit. The skin usually gives more information than people expect, often. Timing adds another important clue for self-checks. Some white spots become obvious in summer because nearby skin darkens while the pale area stays lighter. That happens often with tinea versicolor and pityriasis alba. Some marks stay tiny for years on the shins or forearms after long sun exposure. That points more toward idiopathic guttate hypomelanosis. Some patches enlarge, appear on both sides, or involve white hairs. That should push vitiligo much higher on the list. Age also changes the odds quite a bit. Pityriasis alba appears mostly in children and teenagers.
Idiopathic guttate hypomelanosis becomes more common with age and cumulative sun exposure. Milia can appear at many ages, yet they look like small white beads under the skin. Doctors also ask about itching, dryness, earlier irritation, and recent product use. Those details may sound minor, yet they help explain the picture. The AAD’s phrase “for many reasons” is brief, yet it captures the challenge exactly. Color alone never tells the whole story. Doctors often look at how the spots behave over weeks or months. A condition that stays fixed and tiny suggests one path. A condition that spreads, flakes, or returns every summer suggests another. Even the surrounding skin can offer clues. When nearby skin looks dry, inflamed, or sun-damaged, the contrast can reveal what is happening.
That is why smart observation works better than random treatment. It narrows the field before anything is applied to the skin. It also helps a doctor decide what deserves testing, treatment, or simple reassurance. A good self-check, therefore, starts with five questions. Is the surface smooth or flaky? Are the borders sharp or blurred? Are the spots flat or raised? Did they stand out after sun exposure? Are they spreading, stable, or fading? Those answers cannot replace a diagnosis, yet they create a far stronger starting point than panic ever will. Those basics often prevent several early diagnostic mistakes. Those observations also help patients describe the problem clearly, which often makes appointments faster, more focused, and far more productive.
When a Yeast Overgrowth Changes Skin Color
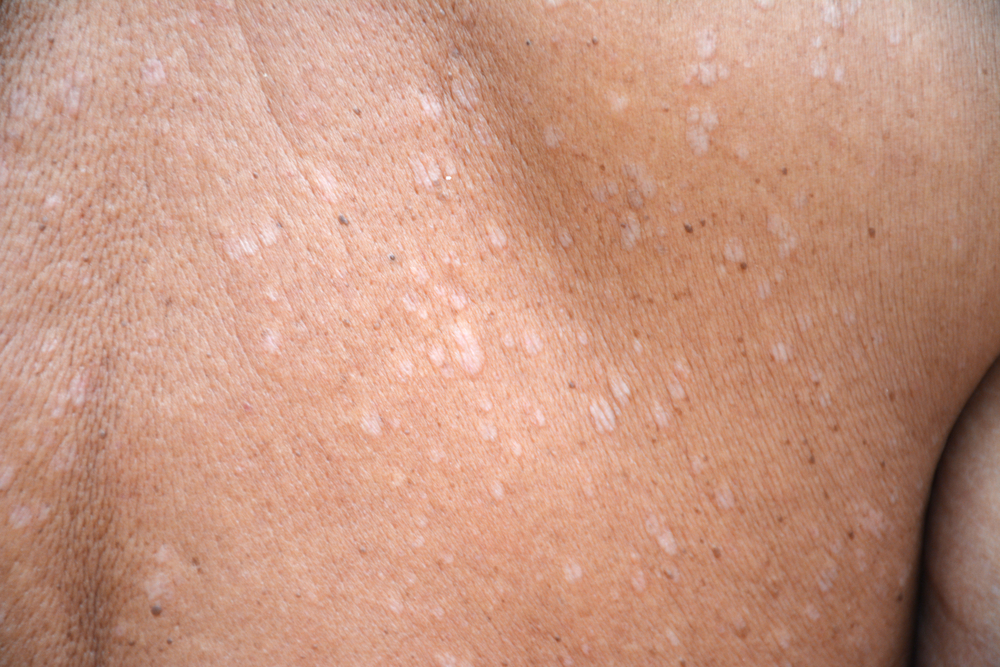
Tinea versicolor is one of the most common reasons pale spots seem to appear after sunny weather. It is also called pityriasis versicolor. The condition develops when yeast that normally lives on the skin grows out of balance. That detail matters because many people attach shame to the word fungal. The NHS says it is “not caused by not washing your skin.” That short line clears up a stubborn myth. The yeast interferes with normal pigment production in the affected areas. As a result, the spots may look lighter, darker, pink, tan, or brown. On darker skin tones, the contrast can look striking. On lighter skin, the change may seem more subtle until tanning begins. The American Academy of Dermatology says the spots can be dry and scaly.
They may also itch, though many people notice color changes first. The upper chest, upper back, neck, and upper arms are the classic sites. That is why white spots on arms often lead doctors to consider this diagnosis early. The patches can start small, then merge into wider, uneven areas. The appearance after sun exposure is one of the strongest clues. Nearby skin tans more normally, while the affected skin does not. That creates a contrast many people notice after holidays or long days outdoors. Doctors may diagnose tinea versicolor by appearance, scale, and body location. A Wood’s lamp can also help in some cases. Treatment usually starts with antifungal shampoo, wash, or cream. When the rash is extensive or keeps returning, tablets may be prescribed.
One practical problem remains after treatment starts. The yeast may clear before the color returns. The AAD explains that pigment can take weeks or months to even out. That delay causes many people to think treatment failed when it did not. Recurrence is also common in warm, humid conditions. Heavy sweating can make repeat flares more likely. That does not mean the condition is dangerous. It does mean the right diagnosis matters. Steroid creams will not solve a yeast overgrowth. A moisturizer alone will not usually fix it either. When pale spots sit on the upper body and show fine scale after tanning, this diagnosis becomes very likely. It is common, treatable, and frustrating, mainly because it can linger cosmetically after the infection itself is controlled.
The condition is especially common in warm, humid regions. The AAD notes that it is one of the most common skin diseases in tropical and subtropical areas. That helps explain why it often returns in hot weather. People who sweat heavily may notice repeat flares. Tight clothing and oily products can also worsen the setting for yeast growth. Even so, the condition stays superficial. It affects the outer skin, not the deeper tissues. That is one reason doctors can usually manage it effectively once the diagnosis is clear. The bigger problem is confusion at home. Many people treat it as eczema first and lose time. Accurate treatment depends on recognizing that color change and infection can linger on different timelines for months.
When the Skin Loses Pigment Completely

Vitiligo becomes a stronger possibility when the skin looks truly white, not simply lighter than usual. The surface usually looks smooth and even. Fine scale is usually absent there. The edges often look crisp and well-defined. This condition develops for a very different reason from tinea versicolor. NIAMS explains that pigment cells are “attacked and destroyed.” Vitiligo is therefore classed as an autoimmune disease. When melanocytes are lost, the skin can turn milky white. The American Academy of Dermatology notes that spots may appear on the face, arms, hands, feet, or legs. Hair, eyebrows, eyelashes, and body hair can also lose color. Some people notice white areas inside the mouth or around the lips. In many cases, patches appear on both sides of the body.
That symmetry is helpful, although not every case starts that way. What usually stands out first is the quality of the color loss. The area often looks clean, smooth, and sharply different from the surrounding skin. Diagnosis relies on history and examination. Dermatologists often use a Wood’s lamp to examine the skin more closely. Both NIAMS and the AAD describe that step in routine evaluation. Doctors may also look for personal or family autoimmune disease. That wider review helps place the skin change in context. Vitiligo is not contagious, and it does not come from poor hygiene. It also will not improve with antifungal products. Treatment depends on the person and the body sites involved. Doctors may use corticosteroid creams, calcineurin inhibitors, or phototherapy.
Some people regain pigment in treated areas. Others need a longer plan with regular follow-up. Sun protection becomes especially important because depigmented skin burns more easily. Tanning can also increase the contrast around the patches. That makes the spots look even more obvious. Vitiligo deserves prompt attention when spots enlarge, match on both sides, or turn nearby hair white. That advice also applies when a smooth white patch appears without any scale or dryness. Here, the aim is not panic or shame. Instead, the goal is clear diagnostic clarity. The course can also change over time considerably. Some people develop only a few areas. Others lose color more widely over months or years. Stress does not cause vitiligo on its own, yet visible changes can cause real distress.
That emotional burden is part of the condition’s impact. Treatment, therefore, focuses on more than appearance alone. Doctors also work to reduce the spread, support repigmentation, and protect affected skin from sunburn. The earlier a person gets a clear diagnosis, the sooner that discussion can begin. That is often more useful than weeks of guessing with over-the-counter products. Vitiligo carries real weight for many people. Early evaluation gives a clearer view of what happens. It also clarifies which treatments may help. Early answers also help families plan treatment, sunscreen use, and follow-up without unnecessary uncertainty or wasted effort later. An earlier diagnosis can also spare wasted treatments. Clear documentation of change over time also helps doctors judge progression, choose treatment sooner, and rule out causes with confidence.
When Dry Skin or Mild Eczema Leaves Pale Patches
Pityriasis alba often causes unnecessary alarm because it can resemble more serious pigment disorders from a distance. It is seen most often in children, teenagers, and young adults. The British Association of Dermatologists calls it a “low-grade eczema.” That phrase explains much of its behavior. Usually, the skin is lighter than the surrounding area, but not always stark white. Its borders tend to look softer than vitiligo borders. Fine scale may sit on the surface, especially early on. The patches may begin slightly pink or dry before they fade to a paler color. The face is the classic location. Even so, the neck, shoulders, and upper arms can also be affected. White spots on arms can therefore reflect mild eczema-related change. It is not contagious either, which reassures many families.
It is also not caused by poor washing. Children with dry skin or atopic dermatitis often develop it more easily. On darker skin tones, the contrast can look much more dramatic. Sun exposure often explains why families notice the patches more in warmer months. Nearby skin tans while the affected area stays lighter. Mayo Clinic notes that a small irritated area can leave a patch lighter than nearby skin. That simple explanation fits pityriasis alba well. DermNet also describes fine scale and pale color as key features. Treatment usually stays simple in most cases. A bland moisturizer, gentle cleansing, and sunscreen are often enough. If the patch is inflamed or itchy, a doctor may recommend a mild steroid cream for a short period.
Patience is often the hardest part. Color often returns slowly, even after the dryness settles. That delay can make parents think something new is going wrong. Usually, the skin just needs more time. Pityriasis alba also does not scar in the usual course. That is reassuring, although the contrast can remain visible for months. Pityriasis alba deserves serious consideration when white spots on the arms appear with dry skin, soft borders, and slight scale. It is a common answer hiding behind a frightening appearance. The most useful response is often steady skin care, sun protection, and medical review if the spots change unusually.
A dermatologist should still assess patches that spread fast, turn sharply white, or stop fitting this typical picture. MedlinePlus also notes that pityriasis alba is common in children and teens. That age group is a useful clue in practice. The patches may feel slightly rough when they first appear. Later, they can look smooth but remain pale. Because the condition is mild, families sometimes stop treatment too soon. That usually does not create harm, yet it can prolong dryness and contrast. Steady moisturizing often works better than short bursts of attention. If the skin stays very dry, fragrance-free products usually help more than harsh cleansers. Those simple steps sound modest, yet they match the ordinary nature of the condition. It is common, mild, and often far less threatening than its appearance suggests to worried families. That perspective alone can calm worried families.
Read More: What Are Those White Bumps That Can Appear On Your Private Parts and What Causes Them?
Tiny White Spots, Tiny Bumps, and the Point to Get Checked
Some white marks are not pigment patches at all. They are tiny bumps or tiny sun-like dots. That distinction changes the diagnosis immediately. Milia belong to the first group. Healthdirect calls them “common and harmless tiny pearly white bumps.” They are small keratin cysts just under the skin surface. They usually appear around the eyelids, cheeks, forehead, or nose. Their raised shape is the clue that matters most. They look like white beads under the skin, not flat areas of color loss. For that reason, milia rarely explain widespread white spots on legs. They can appear elsewhere on the body, though. Most milia need no treatment at all. Picking at them can irritate and leave marks behind. If a white spot is flat instead of raised, another explanation becomes more likely.
Idiopathic guttate hypomelanosis, often shortened to IGH, is one example doctors often consider. DermNet describes it as a benign condition that presents as flat white spots on sun-exposed limbs. That description matches what many adults notice on the forearms and shins. The spots are usually smooth, small, and scattered. Cleveland Clinic says IGH is noncancerous and very common. The spots usually stay stable and usually do not itch. They also do not usually flake. Years of sun exposure seem to play an important role. That is why the lower legs and forearms are such common sites. Compared with vitiligo, the spots are usually much smaller. Compared with tinea versicolor, they lack fine scale and upper trunk dominance. Even with those clues, some situations deserve medical review.
A dermatologist should check spots that spread quickly, crack, itch persistently, turn inflamed, or involve nearby hair whitening. The same applies when white patches become sharply defined or symmetrical. A Wood’s lamp, close examination, and medical history may clarify the cause quickly. The larger lesson is worth keeping in mind. White spots on skin are a description, not a final answer. White spots on arms, white spots on legs, and white spots on the face can arise from very different processes. Tinea versicolor, vitiligo, pityriasis alba, milia, and idiopathic guttate hypomelanosis each leave their own clues. Once the clues are read carefully, the mystery usually starts to shrink. That shift has practical value. It also helps people choose the next step with more confidence.
IGH usually appears in adulthood, not early childhood. That age pattern helps separate it from several other causes. The spots often look like little drops of white paint. They may increase slowly over time, especially on frequently sun-exposed skin. Because IGH is benign, treatment is often unnecessary. Sun protection still makes sense because it helps limit further ultraviolet damage. For some people, reassurance is the main treatment they need. For others, the important step is simply ruling out conditions that need a different response. That is where an experienced skin exam becomes useful. It also reduces the temptation to try harsh products that do not match the real cause. Prompt dermatology review can clarify causes before unnecessary treatments begin.
Disclaimer: The author is not a licensed medical professional. The information provided is for general informational and educational purposes only and is based on research from publicly available, reputable sources. It is not intended to constitute, and should not be relied upon as, medical advice, diagnosis, or treatment. Always consult a licensed physician or other qualified healthcare provider regarding any medical condition, symptoms, or medications. Do not disregard, avoid, or delay seeking professional medical advice or treatment because of information contained herein.
A.I. Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.
Read More: This Ocean Superfood Is Trending in Skincare—But Does It Work?