A fully detailed and comprehensive report on this case study was published in Journal of Central Nervous System Diseases [1].
An unidentified 14-year-old boy from the Midwest – whose family liked to welcome a lot of stray pets – began to display some scary symptoms. He dealt with deep-rooted depression, mood swings, hallucinations, and aggression. He found himself entertaining homicidal thoughts towards the people he cared about, and out of fear for their lives, he became suicidal.
He was diagnosed twice over to be schizophrenic. He was treated for over 18 months for this condition with no signs of improvement. Luckily, a doctor began investigating his case again. It was later discovered that his illness was a result of a bacterial infection in his bloodstream, most likely transmitted through cat scratches.
Early Stage
On both sides of his extended family, there were histories of depression, alcohol abuse, ADHD, and several other disorders. His first episode of depression happened during third-grade where he felt unchallenged but was being bullied for his brilliance. He was placed on an antidepressant medication routine for over year and transferred to a school for gifted kids.
In total, during this ordeal, he endured 4 hospitalizations, several sessions of active therapy, a constant barrage of different combinations of antidepressant and immunosuppressive medications, and severe emotional trauma. The report stated that he developed “psychiatric symptoms including feeling overwhelmed, confused, depressed, and agitated. He said that he was an “evil, damned son of the devil” and wanted to kill himself because he was afraid of his new-onset homicidal thoughts toward those he cared about.”
Initially, He was hospitalized for a week following the display of suicidal behavior. An antidepressant, aripiprazole, was administered to treat his depression, and after he left the hospital, he stopped being suicidal or homicidal.
The Wrong Diagnosis
The boy had to drop out of school in the following months. He was getting so difficult to handle and cater for,
“By December, his illness had progressed in severity, causing his mother to quit her job to provide full-time supervision. In addition to persecutory delusions related to his pets, he developed auditory, visual, and tactile hallucinations and began refusing to leave the house. A second psychiatric hospitalization occurred in December,” the report stated.
In January, the teen developed fresh symptoms that resulted in another hospitalization. He displayed specific somatic symptoms, including excessive fatigue, daily headaches, chest pains, shortness of breath (possible panic anxiety), and urinary frequency. Two psychiatrists later diagnosed him to be schizophrenic and treatments commenced. He was immediately placed on a wide array of medications and was constantly meeting with specialists in psychiatry and other fields. His medications included antidepressants, antipsychotics, and mood stabilizers.
The Truth Discovered
When no improvements were observed, the boy underwent 11 weeks of extensive and advanced testing to determine the actual cause of his condition. The EEGs, MRIs, and several other tests didn’t give the doctors any information worth acting on. They still retained the diagnosis of schizophrenia, and obsessive-compulsive disorder (OCD) was added to it.
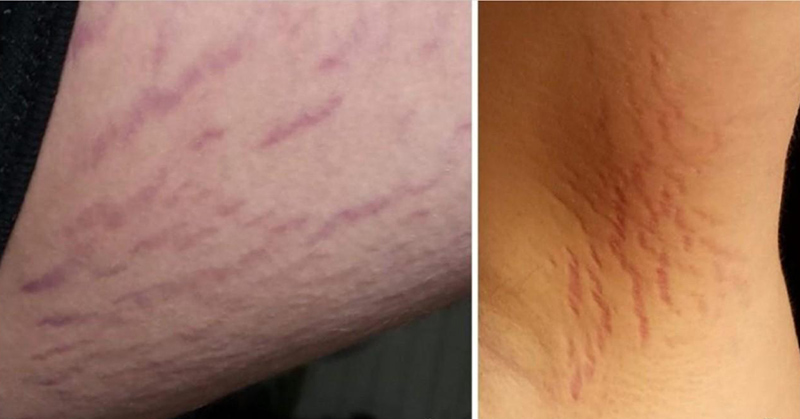
In August of the same year, his parents discovered scarring on his thighs and armpits that resembled stretch marks.
They mentioned this to the doctor who reasoned that he couldn’t have developed stretch marks within that period – he’d been losing weight, not gaining. The boy endured cat bites and scratches prior to the illness, so the doctor this may be linked to his illness.
According to the report “These cutaneous lesions [‘stretch marks’] prompted the attending physician to suspect neurobartonellosis [a bacterial infection] as the cause of pediatric acute-onset neuropsychiatric syndrome in this patient.”
Neurobartonellosis caused by Bartonella henselae bacteria
That actual cause of all the boy’s illness was due to nuerobartonellosis, a bacterial infection caused by the Bartonella henselae bacteria found in a cat’s saliva [2]. The bacteria itself is common and is also carried by healthy cats, but the diseased condition is a rare occurrence. It’s usually transmitted through bites or scratches. The infection affects the nervous system, which most likely prompted the boy’s psychotic symptoms.
Usually, the bacteria can clear on its own, but can sometimes develop into a serious infection. This would require courses antibiotic routines to treat.
“Although causation cannot be established by case reports, microbiological documentation of B henselae bloodstream infection in conjunction with symptomatic improvement during antimicrobial therapy and failure to identify other causes of PANS supports a potential role for neurobartonellosis in this boy’s neuropsychiatric illness,” the report stated.
He was placed on antibiotic treatments for 8 months. He finally tested completely negative for B. henselae in October. After two years of suffering and nearly a year of treatments, he returned to school and his normal life [3].