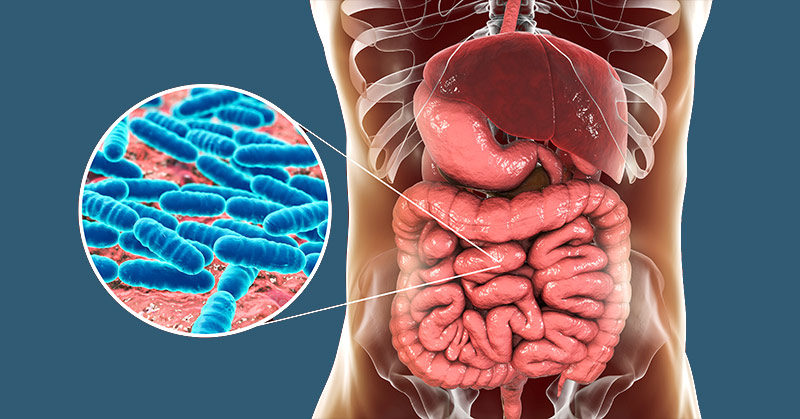
Leaky gut, or “intestinal permeability,” is a fairly new concept in the medical literature that has gained much attention over the last several years. For this reason, many doctors may not have even heard of the condition. The symptoms of a leaky gut, however, can significantly and negatively impact your quality of life. Knowing the symptoms of a leaky gut will help you diagnose it early in order to solve the problem and avoid future health complications.
What is Leaky Gut?
The intestinal lining of your digestive system covers more than four thousand square feet. This lining creates a tight barrier that controls what goes into your bloodstream. A leaky gut occurs when this lining becomes compromised.
An unhealthy gut lining can develop cracks, holes, or separations between the cells (in areas known as tight junctions). This allows partially digested food, toxins, and other substances to travel across your gut lining and into your bloodstream. Your body recognizes these particles as foreign, and launches an immune response, triggering inflammation and changes in the normal bacteria (gut flora) in your digestive tract [1]. An increasing number of studies are now showing that inflammation in the intestinal tract and modifications to your gut flora can lead to a number of diseases.
Read More: Stomach Sounds: Are Yours Normal or Is Something Wrong in Your Gut?
What Causes Leaky Gut?
Medical professionals are still not entirely sure what causes leaky gut syndrome. There is only one thing, as far as scientists know, that regulates intestinal permeability, and that is a protein called zonulin. Two factors can initiate zonulin release: bacteria in your intestines and gluten [2]. Interestingly, some studies have found that gluten only causes intestinal permeability in people with celiac disease or irritable bowel syndrome [3].
The more likely case is that there are multiple factors that can cause leaky gut syndrome. Some of these factors include:
- Eating too much sugar. Diets high in sugar can harm the intestinal wall [4].
- Taking too many NSAIDs. Over time, taking non-steroidal anti-inflammatory drugs (ie- ibuprofen) can increase intestinal permeability [5].
- Drinking too much. Excessive alcohol intake can damage the lining of your gut [5].
- Nutrient deficiencies. Vitamin A, D, and zinc deficiencies may increase interstitial permeability [4].
- Inflammation. Chronic whole-body inflammation can lead to leaky gut syndrome [6].
- Stress. Chronic stress can wreak havoc on your gut, and cause leaky gut syndrome [7].
- Poor gut health. When the balance between the “good” bacteria and “bad” bacteria in your gut is out of balance, it can damage your stomach lining [4].
Is Leaky Gut a Cause or a Symptom?

There is an argument as to whether or not a leaky gut is an underlying cause of chronic disease, or if it is merely a symptom of chronic disease. Currently, there is insufficient evidence to prove that a leaky gut causes any diseases. That being said, there have been some animal studies to show that intestinal permeability was present before the onset of other diseases, such as type 1 diabetes or irritable bowel syndrome [9].
There are also some claims about leaky gut that are not scientifically proven. For example, some people have claimed that a leaky gut causes autism. While there does seem to be a higher proportion of autistic children with intestinal permeability, there is no evidence to suggest that the condition causes autism [10].
What are the Symptoms of Leaky Gut?

The symptoms of a leaky gut are numerous and varied. For this reason, you might dismiss them as being something else. The following complications could be a sign that you have leaky gut syndrome:
1. Skin Problems

Having a compromised intestinal lining could contribute to a number of skin issues, including acne, rosacea, eczema, and rashes. While a leaky gut may not be the sole cause of acne, the inflammation it causes can contribute to skin issues [11].
2. Constipation

If you go days without going to the bathroom or find you have difficulty having a regular bowel movement, it could be because your intestinal lining has been compromised [12].
3. Nutritional Deficiencies
People who suffer from digestive disorders are more likely to be deficient in certain nutrients, such as iron. This is because the villi of your intestinal lining, which are responsible for absorbing nutrients, are damaged [13].
4. Depression and Anxiety

There is growing evidence to support what is called the “gut-brain connection”. This connection is the reason you feel nauseous after giving a big presentation, or why your stomach hurts when you’re stressed. It is possible, then, that intestinal permeability and poor gut health can contribute to mood disorders like anxiety and depression [14].
5. Allergies

When the integrity of your gut flora is compromised, it could increase the passage of pathogens across your gut lining and into your bloodstream. This could then cause an inflammatory reaction and lead to a food allergy [15].
6. Diarrhea

Gas, diarrhea, bloating, and other digestive issues are some of the most common signs of a leaky gut. In fact, a 2015 study found a direct link between intestinal permeability and the progression of irritable bowel disease [16].
7. Insomnia

According to Dr. J. Dreus, PhD, a leaky gut can cause a deficiency in melatonin, the “sleep hormone”. Your gut health can also affect your sleep-wake cycles, which prevents you from falling asleep, or makes it difficult for you to get a restful sleep [17].
Read More: Probiotics & Mental Health: A Guide to Help With Brain, Mood, and Gut Health
8. Infertility

An unhealthy gut microbiome can impair estrogen metabolism and function. This can cause endometriosis, PCOS, endometrial hyperplasia, and infertility [18]. Additionally, women with leaky guts are more likely to have miscarriages [19].
9. Brain Fog

It is possible that a “leaky gut” can lead to a “leaky brain”. If your gut health is compromised, it can cause your brain to feel “foggy”, or for you to have a difficult time concentrating [20].
10. Type 1 Diabetes

Research has found that an abnormal intestinal microbiota, a “leaky” intestinal lining, and altered intestinal immune responsiveness are the “perfect storm” for developing type 1 diabetes. These factors do not mean you will definitely develop type 1 diabetes, but there is a possibility of higher risk [21].
11. Autoimmune Disease
Some studies have shown that intestinal barrier dysfunction may play a role in triggering autoimmune diseases. This is because your immune system will find and attack all of the “escaped particles” that cross your intestinal wall. If you already have a genetic predisposition to autoimmune disease, then a leaky gut puts you at even greater risk [22].
How to Treat Leaky Gut

Typically, treating leaky gut involves removing any foods that cause an adverse reaction until your symptoms go away. The following behaviors may help support a healthy gut:
- Reduce your consumption of added sugars and artificial sweeteners [4]
- Avoid NSAIDs as much as possible [5]
- Consume only moderate amounts of meat, dairy, and eggs
- Eat foods that are rich in prebiotic fiber, like vegetables [4]
- Exercise regularly
- Get adequate sleep
- Reduce stress
- Quit smoking
- Eat more probiotics to boost beneficial bacteria [23]
Many herbal remedies and supplements are available at health food stores claiming that they heal leaky gut. Be wary of these; generally, none of them have been scientifically proven. The best way to heal leaky gut, according to the best current science, is through lifestyle and diet changes. Research into the connection between your gut health and your overall health is ongoing, but nonetheless, it is always a good idea to eat a healthy diet and maintain a healthy gut lining and microbiome.
Read More: Parkinsons and the Gut-Brain Connection
Sources
- “Leaky gut: What is it, and what does it mean for you?” Harvard. Marcelo Campos, MD. November 16, 2021.
- “Intestinal Permeability and its Regulation by Zonulin: Diagnostic and Therapeutic Implications.” NCBI. Alessio Fasano, M.D. August 2012.
- “Rapid disruption of intestinal barrier function by gliadin involves altered expression of apical junctional proteins.” Pubmed. Guy R Sander. August 2005.
- “Intestinal permeability – a new target for disease prevention and therapy.” NCBI. Stephan C Bischoff, et al. November 2014.
- “Intestinal Barrier Function: Molecular Regulation and Disease Pathogenesis.” NCBI. Katherine R. Groschwitz, BS*# and Simon P. Hogan, PhD. December 2014.
- “Systemic inflammation increases intestinal permeability during experimental human endotoxemia.” NCBI. Falco Hietbrink, et al. October, 2009.
- “Stress and the gut: pathophysiology, clinical consequences, diagnostic approach and treatment options.” NCBI. Peter C Konturek, et al. December 2011.
- “Gastrointestinal Candida colonisation promotes sensitisation against food antigens by affecting the mucosal barrier in mice.” NCBI. N Yamaguchi, et al. July 2006.
- “Intestinal permeability defects: Is it time to treat?” NCBI. Matthew A. Odenwald and Jerrold R. Turner. September 2013.
- “Alterations of the intestinal barrier in patients with autism spectrum disorders and in their first-degree relatives.” Pubmed. Laura de Magistris , et al. October 2010.
- “Acne vulgaris, probiotics and the gut-brain-skin axis – back to the future?” Pubmed. Whitney P Bowe and Alan C Logan. January 2011.
- “Epidemiology of constipation in the United States.” Pubmed. A Sonnenberg and T R Koch. January 1989.
- “The gut-brain connection.” Harvard. April 19, 2021.
- “Gut permeability and food allergies.” Pubmed. C Perrier and B Corthésy. January 2011.
- “Intestinal Permeability Regulation by Tight Junction: Implication on Inflammatory Bowel Diseases.” NCBI. Sung Hee Lee. January 2015.
- “Unlocking the Sleep-Gut Connection.” Huffpost. Dr. Michael J. Breus. January 13, 2016.
- “Estrogen-gut microbiome axis: Physiological and clinical implications.” Pubmed. James M Baker. September 2017.
- “Recurrent pregnancy loss is associated to leaky gut: a novel pathogenic model of endometrium inflammation?” NCBI. C. Tersigni, et al. April 2018.
- “Leaky Gut, Leaky Brain?” NCBI. Mark E. M. Obrenovich. October 2018.
- “The “Perfect Storm” for Type 1 Diabetes.” NCBI. Outi Vaarala, et al. October 2008
- “Leaky gut and autoimmune diseases.” Pubmed. Alessio Fasano. February 2012.
- “Systematic review: probiotics in the management of lower gastrointestinal symptoms in clinical practice — an evidence-based international guide.” Pubmed. A P S Hungin, et al. October 2013.