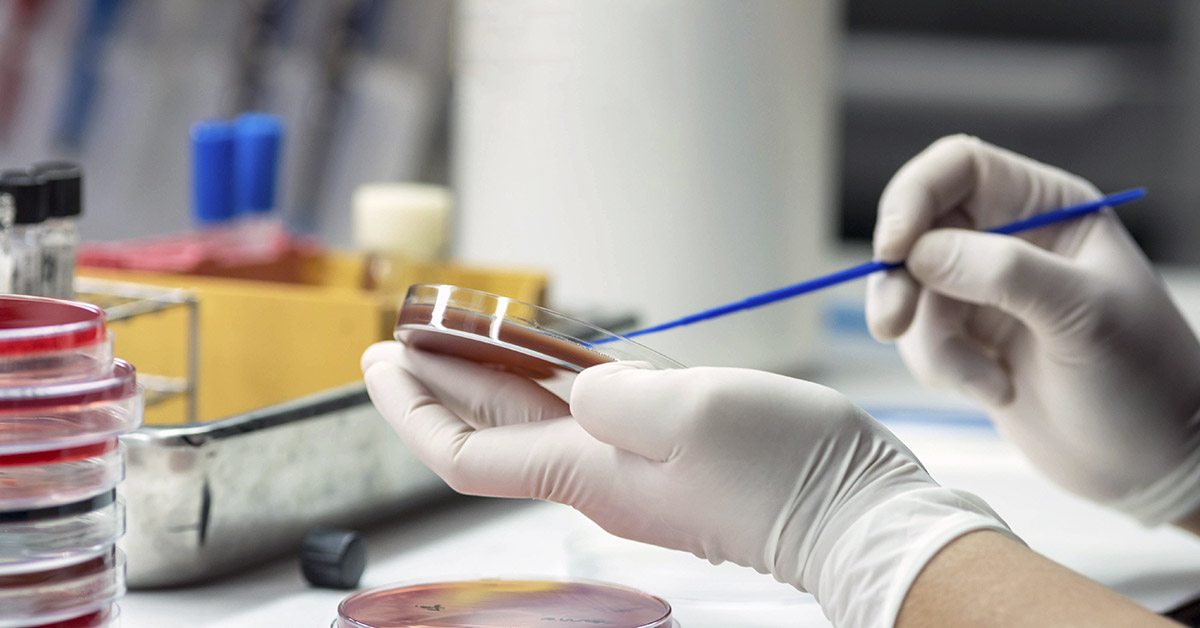
Sepsis is when the body reacts in an extreme way to an infection. It’s dangerous and fatal when not treated in time. Every year, over 1.7 million people in the United States develop sepsis, and at least 270,000 die from it. Doctors still struggle to diagnose this condition that kills more Americans than stroke. Learning and identifying the early signs of sepsis can save lives.
Additionally, it’s important to prevent infections that can lead to sepsis. However, there’s currently no single test for it, so doctors need to uncover the diagnosis through physical exams, medical history, running tests, and their own impressions. In the meantime, technical advancements are working toward creating more accurate and swift assessments to diagnose sepsis. [1]
What is Sepsis?
The immune system protects the body from many ailments, but sometimes it can overreact against an infection. Usually, when there’s an infection, the immune system releases proteins and other chemicals to fight it. However, sepsis occurs when this response becomes extreme and triggers substantial inflammation. The infections that lead to sepsis are usually bacterial.
However, other infections can also cause it — like influenza, fungal infections, and even COVID-19. Although any infection can trigger it, some have a higher risk, like blood poisoning, pneumonia, kidney infections, and abdominal infections. Other common conditions that trigger sepsis include urinary tract infections, appendicitis, infections in the gallbladder, liver, bowels, brains, and spinal cord, as well as infections through wounds or skin inflammations like cellulitis.
Sepsis can happen in a hospital setting, or anywhere else. Sometimes the patient isn’t even aware they have an infection. Sepsis requires immediate treatment since it could deteriorate into septic shock, which often includes plunging blood pressure, organ failure, and major tissue damage. It can become fatal if untreated.
There are three stages of sepsis: sepsis, severe sepsis, and septic shock. Sepsis is when the infection goes into the bloodstream and increases inflammation and blood clotting in the body. Then, severe sepsis occurs when the infection and inflammation worsen enough to inhibit organ function. Septic shock is a severe complication that dramatically lowers blood pressure, which can lead to organ dysfunction, heart failure, respiratory failure, stroke, and even death.
Read More: A woman got the incurable condition ‘cobalt lung’ after vaping marijuana for just 6 months
The Symptoms at Each Stage

Signs of stage one sepsis often include:
- Extreme pain
- Fever and/or chills
- Fast heart rate or low blood pressure
- Sweaty skin
- Confusion or disorientation
- Difficulty breathing
Keep in mind that these symptoms are often mistaken for other conditions, like COVID-19 or pneumonia. They are also hard to identify in infants, young children, and adults with dementia, learning disabilities, or challenges with communication. But if you suspect sepsis, seek medical attention; the faster the treatment, the greater the chance of recovery without lasting complications.
Severe sepsis is associated with organ failure.
https://www.shutterstock.com/image-photo/diagnosis-sepsis-written-on-clipboard-435859072
Therefore, you need one or more of these symptoms to get diagnosed:
- Dizziness
- Difficulty breathing
- Decreased mental ability
- Chills and lowered body temperature
- Skin turning bluish, especially around the lips and digits
- Extreme weakness
- Abnormal heart rate
- Unconsciousness
Septic shock can progress very quickly from sepsis and severe sepsis, becoming even more life-threatening. Signs of septic shock tend to overlap with severe sepsis-like worsened breathing difficulties, blue-tinted skin, and worsened confusion — but it also includes very low blood pressure.
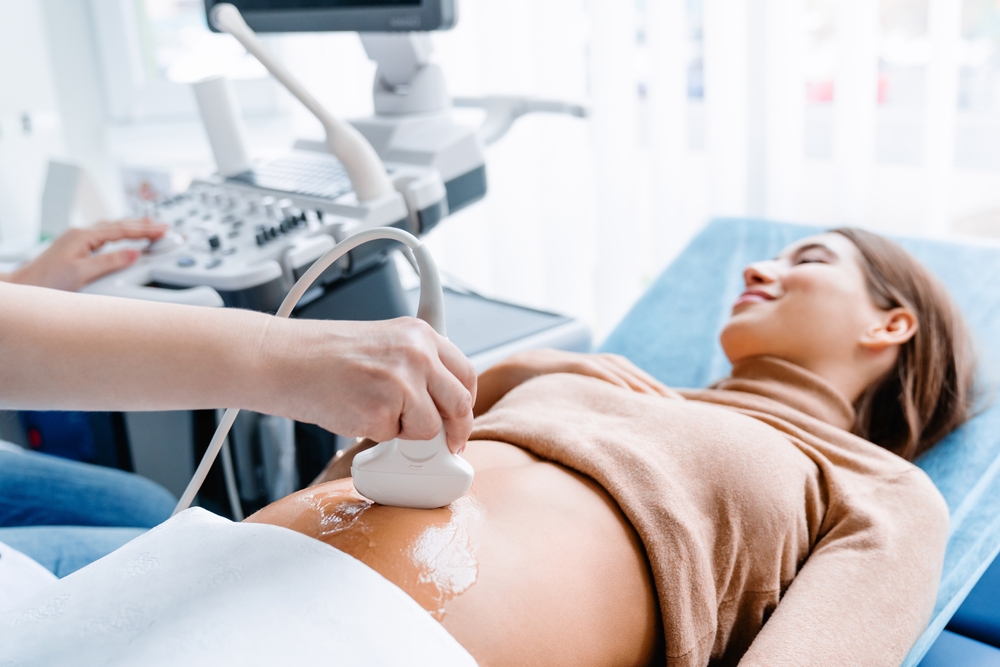
Anyone can get sepsis but those who are at the highest risk include young children, seniors, pregnant women, people with severe injuries or wounds, people with weakened immune systems, those in intensive care units, and those with invasive devices like breathing tubes. Older adults who have chronic illnesses like cancer, high blood pressure, diabetes, and kidney disease are at higher risk, as are those with malnutrition and increased medication usage. Seniors are more likely to have sepsis from common infections. Newborns can get neonatal sepsis during their first month of life through a blood infection. It is the leading cause of infant death although early diagnosis and treatment allows most babies to fully recover.
Maternal screening and neonatal testing have reduced the risk of this occurring.
The symptoms can be subtle but can include:
- Jaundice
- Paled skin
- Not feeding well
- Low body temperature
- Poor circulation and cold extremities
- Listlessness
- Swelling in the abdomen
- Seizures
- Diarrhea
- Vomiting
- Seizures
Read More: Antibiotic use in babies linked to allergies, asthma and other conditions, study finds
Diagnosis and Treatment

If a patient exhibits the symptoms, doctors would check for a low platelet count, a high or low white blood count, acidosis (increased acid in the blood), abnormal liver and kidney functions, and a blood sample testing positive for an infection. Doctors usually try to find the source of the infection and what type it is, using blood tests, urine tests, CT scans, and X-rays. They may give the patient antibiotics. (However, antibiotics won’t help viral infections.) Patients usually need intravenous fluids to prevent a drop in blood pressure; they may also need medications to raise their blood pressure.
Patients with severe sepsis are typically placed in the intensive care unit. Furthermore, those experiencing organ failure require supportive care (like mechanical ventilation or dialysis.) [3] Recovery can take time. The rehabilitation usually begins in the hospital, by slowly moving around and starting to sit up, stand, walk, etc.
After returning home, patients often still struggle with fatigue, lack of appetite, body aches and pains, breathlessness, difficulty moving around, and mental confusion. They may also feel anxious, depressed, and frustrated. Healthcare professionals will help guide the at-home rehabilitation but the plan usually includes eating nutritious food, resting and rebuilding strength, setting small and achievable goals, and getting support from family and friends. While most people recover fully, some have long-term effects like insomnia, nightmares, panic attacks, decreased mental function, organ dysfunction, disabling pain in the muscles and joints, and amputations. [4]
Sepsis Prevention and Technological Advances

To prevent sepsis, one needs to prevent infections whenever possible. Keeping up to date with vaccinations, washing hands properly, and getting routine care for chronic medical conditions can reduce one’s risk of contracting it. Plus, getting immediate medical attention when there might be an infection can prevent sepsis from occurring.
Many researchers are looking into methods of finding sepsis early using technological advancements. For instance, Johns Hopkins researchers are working on a targeted Real-Time Early Warning System, which uses an algorithm to scan hospital electronic records to identify signs to prevent sepsis, alert doctors about at-risk patients, and make way for early treatment. There is also Duke University’s Sepsis Watch algorithm, currently being tried in three hospitals, which uses a deep-learning algorithm. Meanwhile, the CDC has launched a campaign, Get Ahead of Sepsis, to develop tools for tracking the condition, promote early recognition of the symptoms, and prevent infections in the community and medical settings. [4]
Read More: Energy Drinks May Trigger Dangerous Condition in People With Heart Disease, Study
Sources
- “What is Sepsis?” CDC. August 9, 2022.
- “Sepsis Symptoms, Causes and Recovery.” Healthline. Krista O’Connell and Carly Vandergriendt. January 4, 2022
- “Sepsis.” Cleveland Clinic. September 9, 2019
- “I Survived Sepsis. What’s Next?” CDC. August 9, 2022
- “Doctors Still Struggle to Diagnose a Condition That Kills More Americans Than Stroke.” The Atlantic. Simar Bajaj. October 16, 2022