Prescription drugs play an essential role in treating everything from anxiety to chronic illness. But growing evidence shows that some of these more common medications are linked to dementia or memory loss, particularly in older adults. These effects are often linked to how the medications interact with brain chemicals like acetylcholine, which is vital for memory and learning. In some cases, the risk grows with long-term use, high doses, or when multiple drugs are taken together. This does not mean these medicines should never be used – many are life-saving when prescribed correctly. It does mean patients and doctors should carefully weigh risks and consider alternatives. Below are nine medication classes supported by research, along with safer options that may be worth discussing with a healthcare provider.
Benzodiazepines: Calming Drugs With Hidden Cognitive Costs
Benzodiazepines are commonly prescribed for anxiety, insomnia, and seizure control. Popular examples include Xanax (alprazolam), Ativan (lorazepam), Valium (diazepam), and Klonopin (clonazepam). These medications enhance the activity of GABA, a neurotransmitter that slows brain activity, which is why they work as sedatives. While effective in the short term, research suggests long-term use carries significant risks for brain health. One study found that older adults who used benzodiazepines for more than six months had an 84 percent greater chance of developing Alzheimer’s disease. Even moderate use of three to six months increased risk by about 32 percent. Scientists believe these drugs may interfere with memory consolidation and weaken neural pathways over time. Because they are so widely prescribed, their potential impact on dementia rates is concerning.
Exploring Safer Paths for Anxiety and Sleep Problems

There are alternatives that may reduce anxiety or help with sleep without the same dementia risks. Selective serotonin reuptake inhibitors (SSRIs) like sertraline (Zoloft) or citalopram (Celexa) are often prescribed for anxiety and do not carry the same cognitive decline associations. For insomnia, melatonin has been shown in clinical trials to help regulate sleep cycles with fewer side effects. Cognitive behavioral therapy for insomnia (CBT-I) is another option, strongly supported by research, and often more effective than medication in the long run. For some patients, short-term use of benzodiazepines may still be appropriate, but it should be carefully monitored. Safer medications and lifestyle-based therapies offer ways to address symptoms without compromising brain health. Patients should never stop benzodiazepines suddenly but instead work with a doctor on tapering or switching strategies.
First-Generation Antihistamines: Allergy Relief With Cognitive Risks

Older antihistamines, such as Benadryl (diphenhydramine), Chlor-Trimeton (chlorpheniramine), and Tavist (clemastine), are widely used for allergies and sleep. They are known as first-generation antihistamines because they easily cross the blood-brain barrier. These drugs work by blocking histamine receptors but also interfere with acetylcholine, a neurotransmitter vital for learning and memory. That is why they make people drowsy – and also why they can be harmful for long-term brain health. A Georgetown University study found that chronic users of these drugs had a higher risk of dementia compared to those who did not use them regularly. Because many of these products are sold over the counter, people may use them frequently without understanding the risks. Over time, their cumulative effect on memory may be significant, especially in older adults.
Better Evidence-Based Options for Allergies

Fortunately, newer allergy medications are designed to work without the same neurological impact. Second-generation antihistamines such as loratadine (Claritin), cetirizine (Zyrtec), and fexofenadine (Allegra) are less likely to cross into the brain. Clinical studies confirm that these alternatives provide effective allergy relief with fewer sedating or memory-related side effects. Nasal corticosteroid sprays like fluticasone (Flonase) or mometasone (Nasonex) are also considered safe and effective for seasonal allergies. These sprays reduce inflammation in the nasal passages and are often recommended as a first-line therapy. Patients who rely heavily on first-generation antihistamines should consider transitioning to these safer alternatives. By choosing updated treatments, it is possible to manage allergy symptoms without adding unnecessary cognitive risks.
Bladder Antimuscarinics: Relief That May Affect Memory
Bladder antimuscarinics are prescribed to manage incontinence and overactive bladder. Examples include Ditropan (oxybutynin), Detrol (tolterodine), Vesicare (solifenacin), and Enablex (darifenacin). These drugs work by relaxing bladder muscles, but they also block acetylcholine, a neurotransmitter crucial for memory. Blocking acetylcholine in the brain has been tied to confusion, drowsiness, and impaired cognitive performance. A 2015 University of Washington study found that long-term use of these drugs increased dementia risk significantly, especially in older adults. Because bladder problems are often chronic, patients may accumulate years of exposure. This makes antimuscarinics a particularly concerning class of drugs for brain health.
Alternatives to Support Bladder Health Without Cognitive Burden

Pelvic floor exercises, often called Kegels, have been shown in clinical trials to reduce urinary incontinence by strengthening bladder control. Bladder training, which involves scheduling bathroom visits and gradually extending the time between them, is another evidence-based strategy. Botox injections into the bladder muscle can also reduce symptoms and may carry fewer cognitive risks. For some patients, implantable bladder stimulators offer an additional option. While not always suitable for everyone, these approaches allow many to reduce or eliminate reliance on anticholinergic bladder drugs. Discussing these strategies with a healthcare provider may provide safer long-term results. By combining lifestyle adjustments and targeted therapies, patients can often achieve relief without jeopardizing memory.
Antidepressants With Anticholinergic Effects: Mood Treatment at a Cost
Older antidepressants, particularly tricyclic antidepressants such as Elavil (amitriptyline), Tofranil (imipramine), and Pamelor (nortriptyline), are sometimes prescribed for depression or chronic pain. These drugs affect multiple neurotransmitters, including acetylcholine, which is essential for memory and cognitive clarity. Long-term use has been associated with higher rates of dementia in older adults. One large study showed that cumulative exposure to tricyclic antidepressants significantly raised the risk of Alzheimer’s disease compared to non-users. While effective in their time, they are less commonly used today because newer medications have fewer neurological side effects. Still, some patients remain on these drugs for specific conditions. The risks underscore the importance of reviewing antidepressant choices regularly.
Modern Approaches to Treating Depression Safely
Newer antidepressants such as SSRIs, including fluoxetine (Prozac) and sertraline (Zoloft), provide effective treatment without the same anticholinergic burden. SNRIs like venlafaxine (Effexor) are another evidence-based option with less risk of cognitive decline. Cognitive behavioral therapy (CBT) has also been proven effective in treating depression and anxiety, either alone or in combination with medication. Clinical guidelines now often recommend CBT as a first-line treatment, particularly for mild to moderate depression. For patients who do not respond to these approaches, doctors may explore other options such as bupropion (Wellbutrin), which does not have significant anticholinergic effects. By shifting toward these modern treatments, patients can manage mood disorders while protecting long-term brain health. Careful monitoring and open dialogue with physicians are essential when making transitions.
Gastrointestinal Antispasmodics: Digestive Relief With Hidden Risks
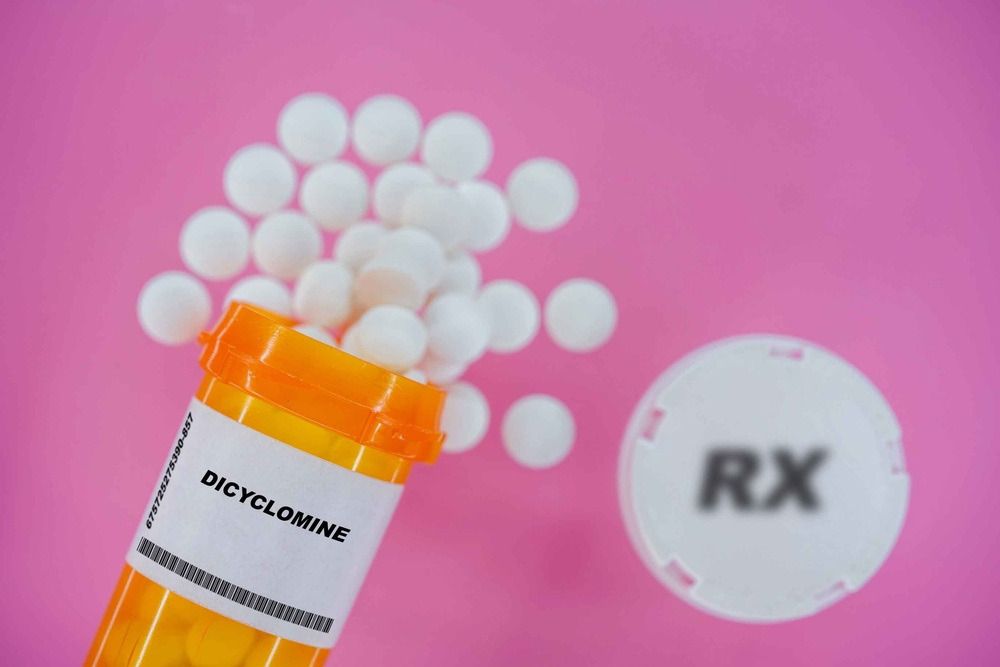
Medications like Bentyl (dicyclomine) and Librax (clidinium-chlordiazepoxide) are prescribed for conditions such as irritable bowel syndrome (IBS). They reduce muscle spasms in the digestive tract, providing relief from cramps and discomfort. However, these drugs also block acetylcholine, the neurotransmitter central to memory and learning. Long-term exposure has been associated with reduced performance on cognitive tests in older adults. Because gastrointestinal disorders often require ongoing management, cumulative exposure can pose long-term risks. While these medications are effective in the short term, their neurological side effects make them less ideal for chronic use. Doctors may recommend them only when other strategies fail.
Evidence-Based Options for Digestive Disorders

Research supports dietary modifications such as the low FODMAP diet, which has been shown in multiple studies to improve IBS symptoms without medication. Probiotics, particularly strains like Bifidobacterium infantis, have demonstrated benefits in reducing bloating and abdominal pain in controlled trials. Stress management techniques, including mindfulness and yoga, are also backed by evidence as helpful in reducing gastrointestinal distress. Fiber supplementation can assist in balancing digestion, especially for those with IBS-related constipation. Combining these approaches often provides relief comparable to medication. Patients should always consult a gastroenterologist to tailor treatment plans. With evidence-based alternatives available, it is possible to support digestive health while minimizing neurological risks.
Antiparkinsonian Agents: Managing Tremors With Tradeoffs

Drugs such as Cogentin (benztropine) and Artane (trihexyphenidyl) are used to ease tremors, stiffness, and rigidity in Parkinson’s disease. These medications act on the nervous system by blocking acetylcholine, improving movement control. However, their anticholinergic effects have been tied to memory decline and confusion in patients. Since Parkinson’s disease already impacts brain function, adding further cognitive strain from medication can complicate care. Studies confirm that patients on anticholinergic Parkinson’s drugs perform worse on memory and attention tests. These medications are usually prescribed when other treatments are not sufficient. Long-term monitoring is essential to balance symptom relief with mental clarity.
Treatment Approaches That Protect Memory in Parkinson’s Disease

Levodopa remains the gold standard treatment for Parkinson’s disease, improving motor symptoms without the same dementia risk as anticholinergics. Dopamine agonists such as pramipexole (Mirapex) or ropinirole (Requip) are also supported by evidence as effective alternatives. Deep brain stimulation (DBS) is another scientifically validated treatment that can reduce the need for medications in certain patients. Physical therapy and regular exercise have been shown in clinical studies to improve mobility and quality of life for Parkinson’s patients. Combining these options often allows patients to reduce reliance on anticholinergic agents. By prioritizing treatments with fewer neurological side effects, patients can better manage both motor function and cognitive health.
COPD and Asthma Anticholinergics: Breathing Easier With a Cognitive Cost
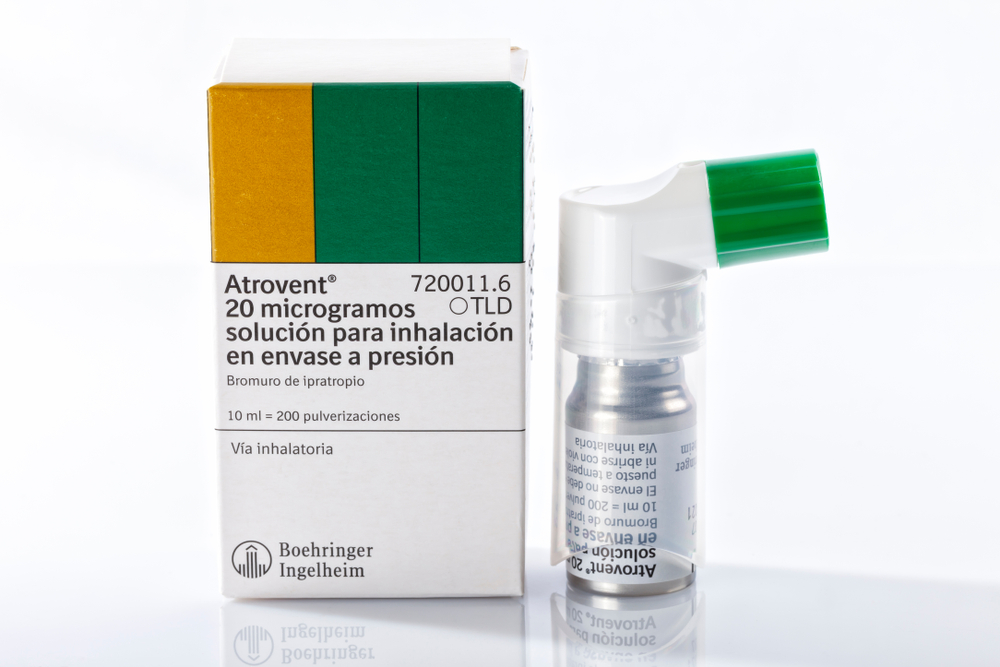
Inhaled anticholinergic medications such as Atrovent (ipratropium) and Spiriva (tiotropium) are commonly used to treat COPD and sometimes asthma. They help open airways by blocking acetylcholine in the lungs, which reduces constriction and eases breathing. While these drugs can be life-changing for respiratory health, long-term studies have suggested that chronic use may slightly increase dementia risk in older adults. The mechanism likely involves cumulative reduction of acetylcholine signaling, which is crucial for memory. Although the risk is not as high as with oral anticholinergics, it becomes more concerning when combined with other medications. Because COPD is a lifelong disease, the potential for cumulative effects grows over time. Patients should work closely with their doctors to balance respiratory needs with brain health.
Respiratory Treatments That Limit Cognitive Risk
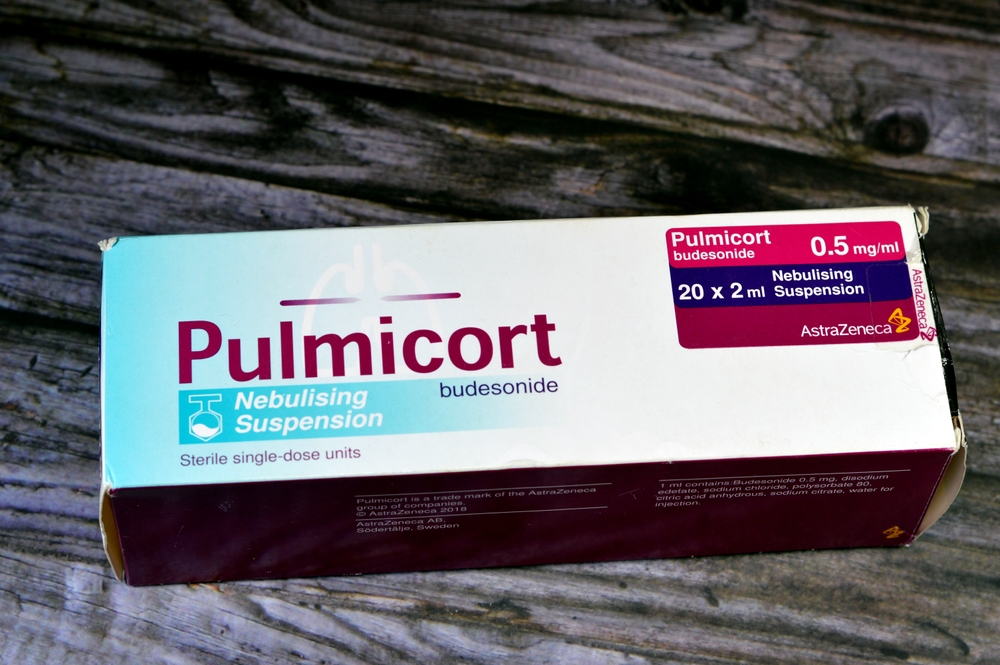
Inhaled corticosteroids such as budesonide (Pulmicort) and fluticasone (Flovent) are often effective for asthma and some COPD patients, with less impact on acetylcholine. Combination inhalers pairing corticosteroids with bronchodilators provide another evidence-based approach. Pulmonary rehabilitation programs, which include exercise training and education, have been shown in studies to improve breathing and reduce flare-ups. Regular physical activity also strengthens lung capacity and improves oxygen efficiency. For some patients, lifestyle measures like quitting smoking and maintaining a healthy weight significantly improve respiratory health. These strategies can reduce the need for long-term reliance on high-risk medications. By blending medical and lifestyle care, patients may breathe easier without increasing dementia concerns.
Motion Sickness Medications: Short-Term Relief, Long-Term Concerns

Drugs for motion sickness and dizziness, such as Transderm Scop (scopolamine) and Dramamine (dimenhydrinate), are widely used for travel and balance disorders. They work by blocking acetylcholine to calm the inner ear and reduce nausea. While useful for short trips, repeated use has been associated with confusion and memory problems in older adults. Because they are available over the counter or by prescription, many assume they are safe for frequent use. Studies have shown that cumulative anticholinergic exposure from these medications adds to dementia risk. Occasional use may not be harmful, but reliance over months or years raises concern. Older adults should be particularly cautious.
Non-Drug Approaches for Motion and Balance Issues

Research supports ginger as a natural option for reducing nausea from motion sickness. Controlled studies have found that ginger capsules can lessen symptoms during travel. Acupressure wristbands, which stimulate pressure points, have also been validated in some trials for reducing dizziness. For individuals with chronic vertigo, vestibular rehabilitation therapy, a form of physical therapy, has been proven effective. These strategies can help patients reduce or avoid repeated reliance on scopolamine or dimenhydrinate. While medication may still be needed in some cases, using non-drug methods first lowers long-term risk. Combining safe natural remedies with therapy offers balanced support for motion-related symptoms.
Ophthalmic Anticholinergics: Eye Treatments That May Reach the Brain
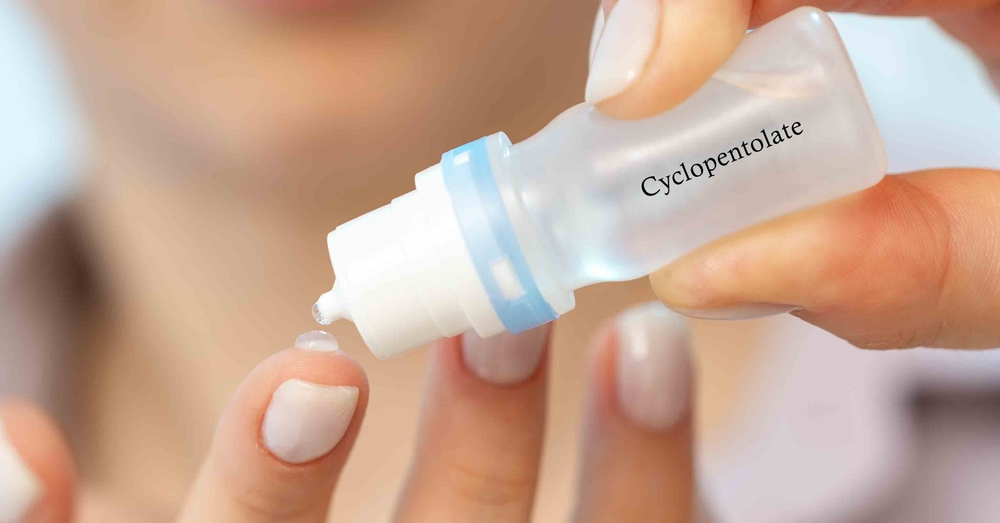
Eye drops like Cyclogyl (cyclopentolate) and Isopto Homatropine (homatropine) are prescribed to dilate pupils or treat certain eye conditions. Although applied locally, these medications can still enter the bloodstream and reach the brain. In older adults, this has been associated with temporary confusion, agitation, and reduced short-term memory. The risk is greater with prolonged or repeated use, particularly when combined with other anticholinergic drugs. Because vision treatments are often repeated over a lifetime, cumulative exposure becomes important to track. While effective for their intended purpose, they should be used with caution in vulnerable patients. Regular monitoring is advised when they are necessary.
Eye Care Options That Minimize Cognitive Impact
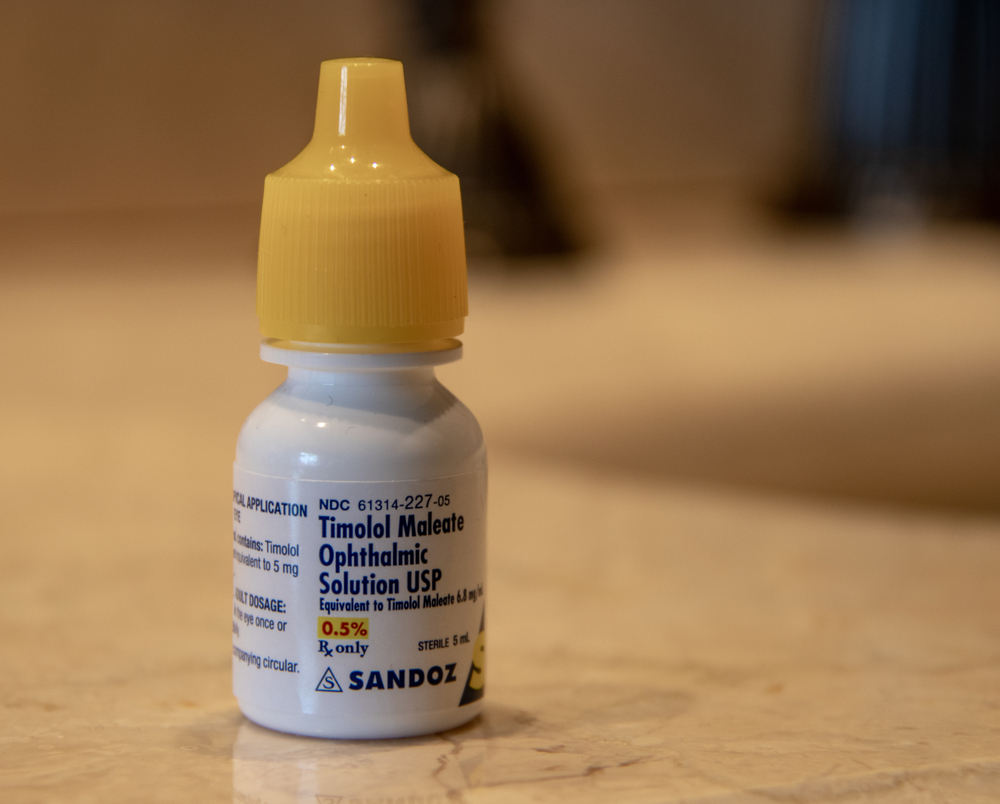
For many patients, shorter treatment courses or lower-strength formulations can achieve the same results with reduced risk. In some cases, non-anticholinergic eye drops or laser treatments may be alternatives for conditions like glaucoma. Studies show that selective beta-blocker eye drops, such as timolol, can lower eye pressure without affecting acetylcholine. For dry eye, preservative-free artificial tears provide relief without systemic effects. Discussing these options with an ophthalmologist ensures both eye health and memory protection. Making careful choices in eye care can help avoid unintended effects on the brain.
Polypharmacy: When Multiple Medications Add to the Risk
Many older adults take more than one prescription at a time, a situation known as polypharmacy. Even if each medication alone carries only a small dementia risk, their combined effects can significantly raise that risk. Research shows that cumulative “anticholinergic burden” – the total impact of drugs that block acetylcholine – is strongly tied to memory decline. In one long-term study, patients using several anticholinergic medications had far higher dementia rates than those using none. Because conditions like bladder issues, allergies, and sleep problems are often treated with these drugs simultaneously, the overlap is easy to miss. Doctors are now urging regular reviews of all prescriptions, especially for patients over 60. Managing the total medication load is just as important as the safety of individual drugs.
Final Thoughts: Balancing Symptom Relief and Brain Health

Medications that block acetylcholine or alter brain signaling are powerful tools in modern medicine. They improve breathing, calm anxiety, relieve pain, and treat many chronic conditions. Yet research consistently shows that long-term use of these drugs may increase the risk of dementia and memory loss, especially in older adults. The key takeaway is not fear, but awareness. Patients should never stop medications suddenly on their own, but instead discuss options and alternatives with their healthcare provider. Safer substitutes exist for many conditions, and lifestyle therapies are supported by scientific evidence as effective complements or replacements. By reviewing medications regularly and seeking out lower-risk treatments, it is possible to protect both current health and long-term brain function. Informed choices today can make a lasting difference in maintaining memory and quality of life.
Read More: Can GLP-1 Drugs Help People Without Diabetes Lose Weight?
Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity. This information is not intended to be a substitute for professional medical advice, diagnosis or treatment and is for information only. Always seek the advice of your physician or another qualified health provider with any questions about your medical condition and/or current medication. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here.

