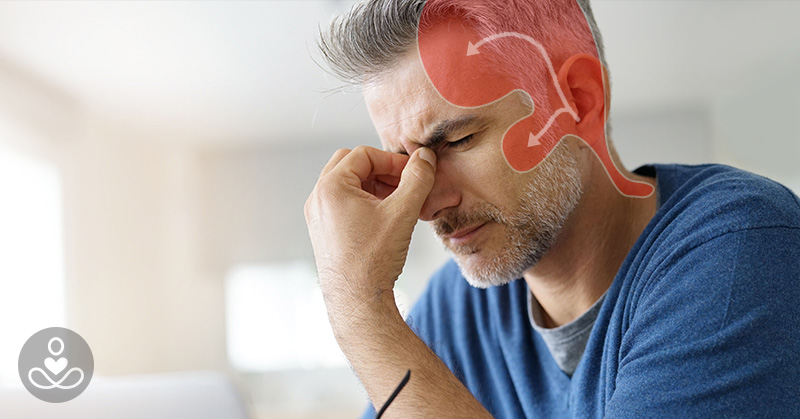
A cervicogenic headache (also referred to as CGH) is a headache classified by a dull pain that starts from the neck and radiates across the back of the head up towards the temples. The pain may even spread across the forehead and around the eyes or ears [1]. Unlike migraines, a CGH isn’t a throbbing pain, and they are almost always one-sided.
Cervicogenic headaches are secondary headaches, meaning there’s an underlying condition that’s causing the pain. The problem usually lies in the neck, but it could also be from the spine or from another condition such as arthritis, cancer, or even an infection. In some cases, a CGH doesn’t require trauma to the neck or spine to exist.
What Causes These Headaches?

Cervicogenic headaches are usually caused by a problem with the neck muscles, which could include overuse of them or even abuse of them. Joints and nerves in the neck could also be causing the headache as could discs. Since all of these are connected, one injury could affect all components [2].
Causes of a CGH could include:
- Trauma
- Whiplash
- Rheumatoid arthritis
- A herniated disk
- Spine degeneration
- Cancer
- Benign tumors
Most people feel a CGH as a steady ache that can become worse when assuming a certain posture or with repeated activities. While both sides of your head may hurt, it’s more common to just experience the pain on one side. However, if the headache is severe enough, the pain may be on both sides.
Read More: Why Do People Get ‘Red Wine Headaches’? (It’s Not the Alcohol)
What a Cervicogenic Headache Feels Like

For some people, the pain of a CGH may start out as intermittent—it’ll come and go. For others, it’s a continuous pain, and for others still, it may start out as intermittent and then progress to more chronic, continuous pain [3].
In addition to neck pain and stiffness along with your headache, you may also experience:
- Pain around your temples or forehead
- Shoulder and arm pain on the corresponding side
- Limited range of motion
More severe symptoms that are less common may include:
- Nausea
- Blurred vision
- Dizziness
- Sensitivity to light and sound
For some people who experience a CGH, they may not even have neck pain per se, but the neck may be tender to the touch or there may be another origin—such as the spine or an infection—that’s causing the cervicogenic headache.
Why a Cervicogenic Headache Isn’t a Migraine

While some of the symptoms of a CGH may resemble those of a migraine or tension headaches, CGHs are not the same as a migraine. In addition to being a non-throbbing pain, cervicogenic headaches almost always involve some type of neck pain, which is uncommon in people who experience migraines. The migraine symptoms we mentioned above—including nausea and sensitivity to light and noise—are rare in people who have a CGH. Evidence shows that migraines and CGHs are two distinct problems and should be approached as such [4].
However, the two do share some similarities as we’ve seen, such as the pain on only one side of the head, and both types of headaches having the potential to worsen without intervention. In fact, CGHs can even happen at the same time as migraine or tension headaches and may even be a possible trigger for them.
Read More: This Hot Water Migraine Trick Can Help Ease Your Headache Without Side Effects
Risk Factors and Diagnosis

Some people who have particular jobs are more at risk to experience CGH due to repeated movements or postures. These people include truck drivers or other drivers, carpenters, and even hair stylists [2].
However, they’re not the only people who are at risk. Other risk factors include:
- Doing strenuous activities such as lifting weights.
- Leaning forward while working on a computer (remember, you should be at a 90-degree angle!)
- Being a woman.
- Assuming any posture that puts more weight on the joints and muscles of the neck, which has the potential to cause CGHs over time.
So how will your doctor know if you’re experiencing a CGH or a migraine? To diagnose a cervicogenic headache, your doctor will conduct a physical exam, review your medical history, and may suggest doing a nerve block test, MRI, CT scan, or x-rays to determine exactly where the pain is coming from [5].
How Are Cervicogenic Headaches Treated?

How your CGH is treated will depend on what’s causing it, so your doctor will want to conduct diagnostic testing before recommending any form of treatment.
Your doctor may recommend physical therapy if your headaches are being caused by a structural problem in the neck [6]. Other research suggests that chiropractic adjustments can be an effective form of treatment for cervicogenic headaches if the headaches are being caused by poor posture or overuse or misuse of the neck muscles [7].
Yoga may also be helpful for people who experience CGHs, particularly with specific exercises [8]. However, as someone who has injured their back a few times doing yoga at home, I’d recommend conducting your practice under the guidance of a professional, especially one that’s experienced in working with people who have cervicogenic headaches! Your medical professional may also prescribe medications or recommend other therapy such as nerve blocks depending on what’s causing your headaches.
When You Need to Seek Help

Since cervicogenic headaches have the potential to be caused by infections or tumors, you should seek a professional medical evaluation for your symptoms. If you have the more severe symptoms of a CGH that we discussed in addition to pain in your arms or tingling sensations in your arms, a fever, seizures, or pain when coughing or sneezing, you should seek medical help as soon as possible [9].
When your body is sending you a message that something isn’t right (pain!), you should always seek the guidance of a medical professional, whether it’s your primary care physician, and integrative doctor, or even another holistic professional. Never ignore your symptoms!
Read More: ‘I Thought I Had A Headache. It Turned Out To Be Herpes (HSV-1) — In My Brain.’
- https://americanmigrainefoundation.org/resource-library/cervicogenic-headache/
- https://www.spine-health.com/conditions/neck-pain/cervicogenic-headache-causes-and-risk-factors
- https://www.spine-health.com/conditions/neck-pain/neck-pain-and-cervicogenic-headache
- https://www.ncbi.nlm.nih.gov/pubmed/1916461
- https://jaoa.org/article.aspx?articleid=2093083
- https://www.medicalnewstoday.com/articles/324108.php
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5525198/
- https://medcraveonline.com/MOJYPT/MOJYPT-03-00050.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3201065/
- https://www.spine-health.com/conditions/neck-pain/neck-pain-and-cervicogenic-headache