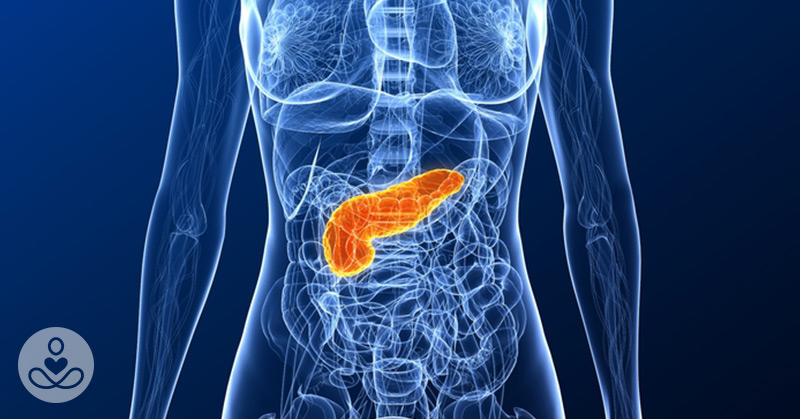
Cancer is ultimately the result of cells that uncontrollably grow and do not die. Normal cells in the body follow an orderly path of growth, division, and death. Programmed cell death is called apoptosis, and when this process breaks down, cancer results. Pancreatic cancer cells do not experience programmatic death, but instead continue to grow and divide. Although scientists do not know exactly what causes these cells to behave this way, they have identified several potential risk factors.
Genes – the DNA type

Cells can experience uncontrolled growth if there is damage or mutations in the DNA, and therefore, damage to the genes involved in cell division. Four key types of genes are responsible for the cell division process: oncogenes tell cells when to divide, tumor suppressor genes tell cells when not to divide, suicide genes control apoptosis and tell cells to kill themselves if something goes wrong, and DNA-repair genes instruct cells to repair damaged DNA.
Cancer occurs when a cell’s gene mutations make the cell unable to correct DNA damage and unable to commit suicide. Similarly, cancer is a result of mutations that inhibit oncogene and tumor suppressor gene functions, leading to uncontrollable cell growth. If you have DNA mutations of oncogenes or tumor suppressor genes that lead to pancreatic cancer, it is likely that the mutation was a result of factors that affected DNA after you were born rather than a result of inheritance from parents.
Read More: Why Didn’t Doctors Caution Patients About the Link Between Hormone Replacement Therapy and Cancer?
Genes – the family type

Cancer can be the result of a genetic predisposition that is inherited from family members. It is possible to be born with certain genetic mutations or a fault in a gene that makes one statistically more likely to develop cancer later in life. About 10% of pancreatic cancers are thought to be caused by inherited gene mutations. Genetic syndromes that are associated with pancreatic cancer include hereditary breast and ovarian cancer syndrome, melanoma, pancreatitis, and non-polyposis colorectal cancer (Lynch syndrome).
Carcinogens
Carcinogens are a class of substances that are directly responsible for damaging DNA and promoting or aiding cancer. Certain pesticides, dyes, and chemicals used in metal refining are thought to be carcinogenic, increasing the risk of developing pancreatic cancer. When our bodies are exposed to carcinogens, free radicals are formed that try to steal electrons from other molecules in the body. Theses free radicals damage cells, affecting their ability to function normally, and the result can be cancerous growths.
Other medical factors

As we age, there is an increase in the number of possible cancer-causing mutations in our DNA. This makes age an important risk factor for pancreatic cancer, especially for those over the age of 60. There are several other diseases that have been associated with an increased risk of cancer of the pancreas.
These include cirrhosis or scarring of the liver, helicobacter pylori infection (infection of the stomach with the ulcer-causing bacteria H. pylori), diabetes mellitus, chronic pancreatitis (inflammation of the pancreas), and gingivitis or periodontal disease.
Read More: Video Shows Immune System Fighting Cancer, and It’s Amazing to Watch
Traits, habits, and diet

Pancreatic cancers are more likely to exist in men than in women, and among African-Americans than among whites. Smoking cigarettes increases one’s risk of pancreatic cancer by a factor of 2 or 3. Even smokeless tobacco has been noted as a risk factor.
Diet and obesity have also been linked to cancers of the pancreas. People who do not exercise much and who are obese are more likely to develop pancreatic cancer. In addition, those who eat diets low in vegetables and fruits and high in red meat and fat are more likely to be diagnosed with the disease. Alcohol consumption is also considered a risk factor for pancreatic cancer. Long-term, heavy drinking leads to chronic pancreatitis, which is a known risk factor for pancreatic cancer.
Symptoms of pancreatic cancer

Cancer symptoms are quite varied and depend on where the cancer is located, where it has spread, and how big the tumor is. Pancreatic cancer is often called a “silent” disease because it rarely shows early symptoms and presents non-specific later symptoms. Tumors of the pancreas cancers are usually too small to cause symptoms. However, when the cancer grows, symptoms include:
- Pain in the upper abdomen from the tumor pushing against nerves
- A painless yellowing of the skin and eyes and darkening of the urine called jaundice, is created when the cancer interferes with the bile duct and the liver.
- Loss of appetite, nausea, and vomiting
- Significant weight loss and weakness
- Acholic stool (pale or grey stool) and steatorrhea (excess fat in stool)
These symptoms of pancreatic cancer have numerous other causes, making it difficult to diagnose the disease before it is in an advanced stage. Cancers of the pancreas are also associated with Trousseau’s sign – spontaneous blood clots formed in the portal blood vessels, deep veins of the arms and legs, or other superficial veins. Clinical depression is another symptom that is sometimes reported before the cancer is diagnosed.
If the cancer spreads or metastasizes, additional symptoms can present themselves in the newly affected area. Symptoms of metastasis ultimately depend on the location to which the cancer has spread. Islet cell or neuroendocrine cancers of the pancreas may cause the organ to produce too much insulin or hormones. This may lead to weak or dizzy feelings, chills, muscle spasms, or diarrhea.

Read More: 20-Year-Old Takes On Raising Her Five Siblings After Both Parents Die From Cancer