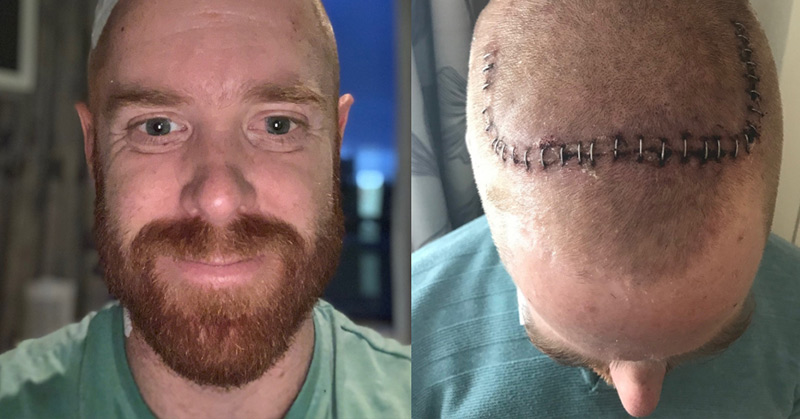
Todd Murfitt hadn’t been expecting to sit 20 minutes at the doctor’s office and be diagnosed with Young Onset Parkinson’s disease.
The high school principal at St John the Baptist Primary School in Adelaide, Australia, was 35 when he received the shocking news. He’d suddenly began to notice violent and unusual tremors in his fingers while he typed, and he certainly hadn’t been expecting it to be anything serious.
“I turned up at the neurologist appointment not really knowing what to expect, certainly not expecting any big news,” he said to ABC News [1]. “It was a bit of a surprise to find out, after a 20-minute consult, that the neurologist was fairly certain I had young-onset Parkinson’s.“
According to Murfitt, who is a father of two, his symptoms included a persistent ringing in his ears, loss of motor control, internal and external tremors.
Two years down the line, Murfitt’s condition worsened progressively with his motor functions deteriorating rapidly. His medications were no longer effective, and so the doctors recommended Deep Brain Stimulation, an alternative targeted treatment which gave him back his life to a great extent.
Murfitt’s pace-making surgery
Deep Brain Stimulation (DBS) is a surgical procedure which is used to treat the motor-related symptoms of several neurological conditions, the most common of which is Parkinson’s disease. The surgery is usually performed as an awake craniotomy, which means the patient can be awake and locally anesthetized for the operation, although he’d still be able to feel a bit of pain from prods and pokes.
The surgery involves the surgical implantation of tiny electrodes into the parts of the brain that control motor function [2]. These electrodes would transmit signals from a computer chip to which they are connected by an under-skin wire. Upon activation, the electrodes would begin to painlessly transmit signals that would stimulate the concerned parts of the brain to reduce the motor-related symptoms of the disease.
Murfitt was a good match for the procedure due to his relatively young age and absence of dementia, which could be worsened by DBS [3].
Murfitt was shocked at how his condition further deteriorated when he was taken off his meds in preparation for the procedure. His family, friends, neighbors, and community raised over $40,000 to cover the bills, a gesture he would be eternally grateful for. To express their full support, his three brothers and niece shaved their heads to match his, right in the presence of the kids at his school.
“My girls were sitting there and instead of seeing dad sitting there getting his head shaved for surgery, they saw their uncles, they were sitting with their cousins and it was just fun,” Mr. Murfitt said.
New technologies introduced, grounds broken with Murfitt’s surgery
Performing DBS as an awake craniotomy can be challenging, much like other procedures, but it’s important for the patients to update the surgeons on the sensations they are experiencing. This enables the doctors to position the electrodes at the most vital and essential locations. Close to the collarbone in the chest cavity, a small chip device known as a pulse generator is implanted to generate the stimulating signals transmitted by the electrodes.
According to neurologist Dr. Rob Wilcox, one of the surgeons who operated on Murfitt, DBS is a pacemaker for the brain. He explained that the procedure involved dedicated teamwork and was aided by the fact that Murfitt is still young. Dementia is not a good fit for DBS. Also, his age would allow them to record and track his progress over a long period of time.
“I’m the sort of navigator and Dr. Matt McDonald is the pilot, I do the electrical signals and targeting, Dr. McDonald does the surgery, and the third member of the team is the patient,” Dr. Wilcox said.
Murfitt is the first DBS patient to be treated with directional wires as against the traditional ring system. Directional wires or steerable leads for implantation is an advanced technology that enables signals to be directed more precisely, channeling them in accurate shapes and ranges directly to the desired parts of the brain with more control.
Since the brain shrinks as age progresses, the wires can have to be changed periodically. When Murfitt would go in his for his periodic check-ups, the doctor would read the information on his brain activity from a Bluetooth device connected to his chest chip, which would receive data from the directional leads.
“The brain wires that have been around for some time are called ring electrodes, four rings with each electrode going into the brain,” Dr. Wilcox explained. “The difference between steerable or directional leads is the ring has been split into three different segments and so electricity can be pushed forwards, or to the side and out, or to the side and in, or both sides.”
Getting back on his feet
Murfitt described the sensations he experienced during the surgery as “overwhelming”. He could finally feel control of his body gradually returning to him.
“I was just flabbergasted because, despite the pain of needles and things like that, the overwhelming sense was wow, it feels like a new body, I can’t believe it. Having gone through it, I would go through that again weekly, just to feel the way I do at the moment,” Murfitt said.
He testified to the fact that the procedure is significantly more effective than the medications, and it would allow him to live a better, healthier, and happier life.
“I always felt like I was still a good dad but now I feel like I can really do that, I feel completely unrestricted,” he said. “I can have so much more quality time with the girls. It’s just great.”
He’s now a member of the Parkinson’s Community and while he’s still in recovery, it’s easier to have people with similar experiences to connect with.
“There’s been one person who’s gone through DBS that’s been really helpful,” he explained. “What I noticed the whole time was that there was never a flicker of doubt that she might have done the wrong thing, there’s no regret and I can see where that comes from.”
More about Young Onset Parkinson’s disease (YOPD)
About 10 to 20 percent of people with Parkinson’s develop symptoms before age 50, which is described as ‘young onset’ [4]. It’s not easy to make a straight diagnosis of YOPD. The condition is rare and often misdiagnosed as stress symptoms, muscle damage, fatigue, and other conditions that affect motor function. The actual cause of YOPD is unknown, but it’s believed to be caused by genetic and environmental factors affecting the central nervous system.
Symptoms include tremors in the face, hands and legs, rigidity of the limbs, falls, dystonia (painful muscle contractions that may distort posture), dyskinesia (abnormal impairment of voluntary movement), and total loss of motor control as the disease progresses [5]. The non-motor symptoms include depression, anxiety, mood swings, delusions, and hallucinations, although the younger patients are less likely to suffer these symptoms and signs of dementia.
Treatment options for Parkinson’s disease are essentially the same despite the age at which it is discovered, except for DBS which isn’t suitable for older patients. Medications are usually administered before surgery is considered an option. Medications include Amantadine for increased secretion of dopamine and reduction of dyskinesia, MAO-B inhibitors for better utilization of dopamine, and anticholinergic drugs for tremor control.
DBS is a procedure usually suggested when the patient’s condition is advanced. Lesioning surgeries have become less popular with the advancement of DBS [6]. Lesioning involves destroying the parts of the brain that contribute to the symptoms, and it’s rarely performed anymore.
Sources
- Frost & Prosser. Adelaide man receives ‘pacemaker for the brain’ to combat young onset Parkinson’s disease. ABC News. https://www.abc.net.au/news/2019-06-04/man-receives-pacemaker-for-the-brain-to-combat-parkinsons/11173400?fbclid=IwAR066PNaGUIEpUa-IlFIBQWkcwD0pir5wgr1bLnDEietk1V5SC9fHIHH5aU. Retrieved 10/06/19
- Deep Brain Stimulation. Adelaide NeuroSpine. https://www.adelaideneurospine.com.au/deep-brain-stimulation/. Retrieved 10/06/19
- Inacio, Patricia. Deep Brain Stimulation May Increase Dementia Risk in Some Parkinson’s Patients, Study Suggests. Parkinson’s News Today. https://parkinsonsnewstoday.com/2019/02/01/deep-brain-stimulation-increased-risk-dementia/. Retrieved 10/06/19
- Young-Onset Parkinson’s Disease. Michael J. Fox Foundation. https://www.michaeljfox.org/news/young-onset-parkinsons-disease. Retrieved 10/06/19
- Young Onset Parkinson’s. Parkinson’s Foundation. https://parkinson.org/Understanding-Parkinsons/What-is-Parkinsons/Young-Onset-Parkinsons. Retrieved 10/06/19
- Surgical Treatments for Parkinson’s Disease. Parkinson’s News Today. https://parkinsonsnewstoday.com/parkinsons-disease-treatments/surgical-treatments/. Retrieved 10/06/19
- Young-onset Parkinson disease. Orpha. https://www.orpha.net/consor/cgi-bin/OC_Exp.php?Lng=EN&Expert=2828. Retrieved 10/06/2019
- Staff Writer. Deep Brain Stimulation. Mayo Clinic. https://www.mayoclinic.org/tests-procedures/deep-brain-stimulation/about/pac-20384562. Retrieved 10/06/19
- Awake craniotomy. University Hospital Southampton. https://www.uhs.nhs.uk/OurServices/Brainspineandneuromuscular/Neurosurgery/Diagnosisandtreatment/Braintumours/Awakecraniotomy.aspx. Retrieved 10/06/19
- DBS with Directional Lead Technology. University of Pittsburgh. https://www.neurosurgery.pitt.edu/centers-excellence/epilepsy-and-movement-disorders-program/dbs-directional-lead-technology. Retrieved 10/06/19
- Amantadine for Treating Parkinson’s Disease. Stanford Health Care. https://stanfordhealthcare.org/medical-conditions/brain-and-nerves/parkinsons-disease/treatments/amantadine.html. Retrieved 10/06/19
- What are MAO-B inhibitors? Parkinson’s Disease. https://parkinsonsdisease.net/medications/mao-b-inhibitors/. Retrieved 10/06/19
- Anticholinergic Drugs. Parkinson’s. https://parkinson.org/Understanding-Parkinsons/Treatment/Prescription-Medications/Anticholinergic-Drugs. Retrieved 10/06/19