Rheumatoid arthritis (RA) is an autoimmune and inflammatory disease, where the immune system attacks healthy cells in the joints. This causes the joints to become inflamed, painful, unsteady, and deformed. Not much is known about what causes this autoimmune reaction, and there is currently no cure, although there are many strategies to help manage the condition. However, researchers at the University of Colorado School of Medicine have discovered a bacteria in the gut that may trigger the disease in people at risk of autoimmune conditions.
Bacteria That May Cause Rheumatoid Arthritis
Researchers have studied rheumatoid arthritis for years, with a particular focus on the antibodies that attack the joints and cause this condition. Past research indicates that these antibodies can form around the body — especially in areas like the intestines, lungs, and mouth — for 10 years before any symptoms of RA appear. So this new study examines why these antibodies are found in these areas and how they are triggered.
Kristine Kuhn, MD, Ph.D., associate professor of rheumatology, and a team of researchers studied the antibodies taken from the bodies of people with blood markers indicating they were at risk for RA. Then they mixed these antibodies with the feces of these at-risk people to pinpoint the bacteria the antibodies were meant to target. Next, the team placed this bacteria in mice, and sure enough, they began to develop the same blood markers as the people at risk. Not only that, they began to actually develop RA.
This helped confirm the hypothesis that specific gut bacteria triggered the production of antibodies that cause RA. The scientists reasoned that although the antibodies are meant to attack this bacteria, they cause rheumatoid arthritis when they expand outside of the intestines and attack the joints. The bacteria also can activate immune cells called T cells in people with RA. T cells work with different inflammatory responses in the body and have been linked to other autoimmune diseases.
Read More: Do These Hand Exercises In The Morning to Relieve Arthritis Pain In Your Wrists and Fingers
Learning More About the Bacteria
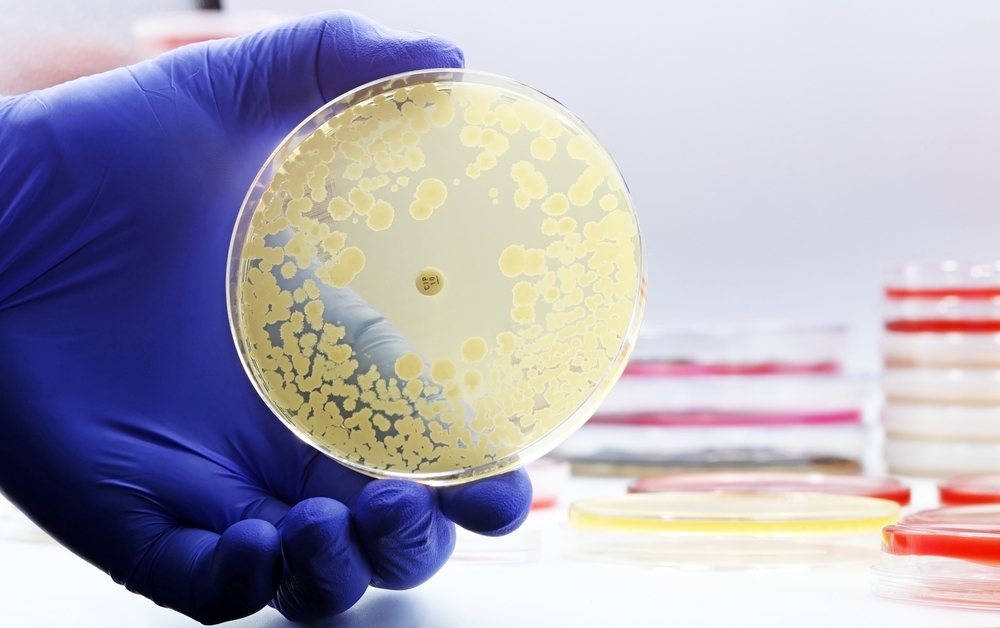
This bacteria was found in 20% of people diagnosed with RA or have antibodies that cause RA. However, it hasn’t been found in the feces of healthy people with no risk, and so far, it’s unclear how common this bacteria is for the general population. “Through studies in humans and animal models, we were able to identify these bacteria as being associated with the risk for developing RA,” Kuhn says. “They trigger an RA-like disease in the animal models, and in humans, we can show that this bacterium seems to be triggering immune responses specific to RA.” [1]
This study shows promise for developing treatments for people with RA

First, the researchers need to better understand this bacteria, if it has any correlations with genetic or environmental factors, or if it correlates with other immune responses. “Then we could say, ‘This is a marker that’s useful in helping predict who will go on to develop RA,’ and apply prevention strategies,” says Kuhn. “The other opportunity there is that if we can understand how it is triggering these immune responses, we might be able to block the bacteria’s ability to do that.” This study brings hope that RA will one day be curable and perhaps even preventable after further research. [2]
Read More: Skeletons Say Osteoarthritis Isn’t About Aging, It’s About Activity
More About Rheumatoid Arthritis
There are about 1.5 million people in the United States with RA, according to the Arthritis Foundation. [3] Current treatment for RA is most effective when the disease is diagnosed early. Therefore, it’s important to be familiar with the symptoms. Overall, RA is a chronic illness noted for its inflammation and pain in the joints. It commonly appears around the hands, knees, feet, and wrists.
However, it can also appear throughout the body, like in the lungs, eyes, or heart. The symptoms can ebb and flow, going through periods of worsened pain, called flares or exacerbations. Sometimes, there are periods of remission when the pain can disappear. Even though the signs can come and go, don’t ignore them; seek early treatment. [4]
The symptoms include:

- Pain or aches in multiple joints
- Stiffness or swelling in multiple joints
- Joint symptoms mirrored on both sides of the body
- Loss of joint function and deformities
- Fatigue
- Loss of appetite
- Low-grade fever
Risk Factors and Treatment
There are many risk factors for developing RA. The disease tends to appear among adults in their 50s or older, and women are two or three times more likely to develop it than men. Also, people with certain genes are predisposed to RA, especially when they are obese or smoke. Similarly, people who smoke are at high risk, as well as children who were exposed to second-hand smoke. A poor diet with high consumption of sugar, sodium, iron, and red meat, as well as obesity, comes with an increased risk.
There is currently no cure for RA. However there are treatments to manage the symptoms, prevent further damage, and improve quality of life. Treatment plans vary depending on each case, but they can include: medications, dietary and lifestyle changes, certain exercises, and alternative or home remedies. Once people with RA find a helpful treatment, they are able to live an active life with reduced risk of complications. [5]
Read More: Could Exercise Prevent Arthritis? New Research Is Hopeful
Sources
- “Can gut bacteria cause rheumatoid arthritis?” Science Daily. University of Colorado Anschutz Medical Campus. October 26, 2022
- “Newly discovered species of bacteria in the microbiome may be a culprit behind rheumatoid arthritis.” The Conversation. Meagan Chriswell. October 27, 2022
- “Rheumatoid Arthritis: Causes, Symptoms, Treatments and More.” Arthritis Foundation. October 15, 2021
- “Everything You Want to Know About Rheumatoid Arthritis.” Healthline. Nancy Carteron, MD.D, FACR November 23, 2021
- “Rheumatoid Arthritis.” Cleveland Clinic. February 18, 2022

